Where Do We Perform Prostate Biopsy
Prostate fusion biopsy is performed at the HIFU CLINIC Prostate Cancer Treatment Center at Carolina Medical Center, one of the most modern hospitals in Poland.
HIFU CLINIC Prostate Cancer Treatment Center is the only medical center in this part of Europe that utilizes the Koelis Trinity fusion biopsy system the most modern specialist equipment in this part of Europe .
Watchful Waiting Or Active Surveillance
Your doctor might suggest waiting to see if your tumor will grow or spread before you treat it. Most prostate cancer grows slowly. Some doctors think itâs better not to treat it unless it changes or causes symptoms. In watchful waiting, your doctor will closely track how the disease makes you feel. With active surveillance, youâll also get regular tests to check on the cancer.
Also Check: External Beam Radiation Treatment For Prostate Cancer
Preparation For The Biopsy
Patients who received anticoagulant therapy were consulted to relevant disciplines, and acetylsalicylic acid, anticoagulants were discontinued 7, and 3 days before biopsy, respectively. Excluding patients requiring intervention because of development of bleeding episodes, anticoagulant therapy was reinitiated on the postprocedural first day. In all cases, before biopsy as antibiotic prophylaxis 500 mg ciprofloxacin was given twice daily for 2 days. To prevent voiding dysfunction, the night before the biopsy alpha-blocker therapy was initiated, and continued further for 30 days. For rectal cleansing the night before the biopsy patients used rectal enemas. All cases were informed in detail about the procedure, and their written informed consent forms were obtained.
Read Also: Fla Treatment For Prostate Cancer
Possible Harms From Diagnosis
Screening finds prostate cancer in some men who would never have had symptoms from their cancer in their lifetime. Treatment of men who would not have had symptoms or died from prostate cancer can cause them to have complications from treatment, but not benefit from treatment. This is called overdiagnosis.
Prostate cancer is diagnosed with a prostate biopsy. A biopsy is when a small piece of tissue is removed from the prostate and looked at under a microscope to see if there are cancer cells. Older men are more likely to have a complication after a prostate biopsy.
A prostate biopsy can cause
- Pain.
- Blood in the semen or ejaculate.
- Infection.
How Doctors Determine Whether To Recommend A Prostate Biopsy

No two patients are alike, and a urologist needs to take many variables into account before recommending a prostate biopsy, including a patients:
- Age and life expectancy
- Comorbidities
- Change in PSA values across time.
The decision of whether to undergo a prostate biopsy should be determined after an individual conversation with your doctor during which he or she presents you with the big picture of your situation.
Compare, for example, the case of two 50-year-old men: One of them has been diagnosed with heart failure and is in poor overall health. The other has no pre-existing health conditions. I probably wouldnt advise a prostate biopsy for the 50-year-old with heart failure because prostate cancer is unlikely to cause his death within the next five years.
But I would recommend that the healthy 50-year-old get a prostate biopsy, because even if his cancer isnt aggressive right now, missing a prostate cancer diagnosis may result in his death from the disease in 15 years. In his case, it would be better to risk the prostate biopsy to catch the cancer early and improve his chances of long-term survival.
Read Also: Prostate Cancer T1c Gleason 7
What Is An Mri Fusion Biopsy Of The Prostate
The MRI/US fusion biopsy is a revolutionary diagnostic tool for prostate cancer screening that combines MRI with ultrasound technology to pinpoint the precise areas of suspicion where biopsies should be taken. Not only does this offer more accurate, reliable results in the detection of prostate cancer, but it also reduces the risks and side effects associated with blind sampling. Dr. Ali Kasraeian is highly experienced and knowledgeable in this advanced technique, having been the first practice in the Greater Jacksonville area to offer MRI fusion biopsy.
Top 10 Wedding Photographers In Richmond Va
Whether youre after bold and creative or softly-toned and whimsical, theres a wedding photographer out there to suit you. Couples getting married in Virginia will find theres no shortage of outstanding photographers calling the state home.
Read on to check out our comprehensive list of the top wedding photographers in Richmond. Read on to view their portfolios, see a little about their personalities, and evaluate their services for your big day.
Recommended Reading: How Do Guys Get Prostate Cancer
What Is A Transperineal Biopsy
This is where the doctor inserts the biopsy needle into the prostate through the skin between the testicles and the back passage . In the past, hospitals would only offer a transperineal biopsy if other health problems meant you couldnt have a TRUS biopsy. But many hospitals have stopped doing TRUS biopsies and now only do transperineal biopsies.
A transperineal biopsy is normally done under general anaesthetic, so you will be asleep and wont feel anything. A general anaesthetic can cause side effects your doctor or nurse should explain these before you have your biopsy. Some hospitals now do transperineal biopsies using a local anaesthetic, which numbs the prostate and the area around it, or a spinal anaesthetic, where you cant feel anything in your lower body.
The doctor will put an ultrasound probe into your back passage, using a gel to make this easier. An image of the prostate will appear on a screen, which will help the doctor to guide the biopsy needle.
If youve had an MRI scan, the doctor may just take a few samples from the area of the prostate that looked unusual on the scan images. This is known as a targeted biopsy.
What You Should Ask Your Doctor Before Your Prostate Biopsy
Dr. Klein recommends asking your physician these questions ahead of time:
This article originally appeared in Cleveland Clinic Mens Health Advisor.
Also Check: What Are The After Effects Of Radiation For Prostate Cancer
What Is A Prostate Fusion Biopsy
Prostate fusion biopsy is a procedure in which tiny samples of the prostate gland tissue are collected. The collected samples are then evaluated by an experienced pathomorphologist under a microscope, often with the addition of various immunohistochemical dyes.
Prostate fusion biopsy is performed through the perineum with the use of a TRUS image and a magnetic resonance image. The procedure is carried out by a urologist and a radiologist assisted by a nurse. Fusion biopsy is based on the fusion of multiparameter magnetic resonance images and real time ultrasound imaging.
Since 2015, the European Association of Urology recommends that every repeated prostate biopsy should be carried out based on the mpMRI examination and any abnormalities found in it. From 2019, the European Association of Urology also recommends that every patient who is considered to undergo prostate biopsy should consider undergoing a prostate MRI first. Magnetic resonance imaging is performed specifically for the purpose of a subsequent prostate fusion biopsy.
Biopsy During Surgery To Treat Prostate Cancer
If there is more than a very small chance that the cancer might have spread , the surgeon may remove lymph nodes in the pelvis during the same operation as the removal of the prostate, which is known as a radical prostatectomy .
The lymph nodes and the prostate are then sent to the lab to be looked at. The lab results are usually available several days after surgery.
Read Also: What Is A Good Psa Reading For Prostate
Additional Tests That May Aid Prostate Cancer Diagnosis
There are few other diagnostic tools or tests, which can be performed before you have a prostate biopsy, that may help your physician gather more information about your specific case. These procedures may help determine the likelihood of the presence of cancer and its aggressiveness and increase the accuracy of a biopsy when performed. Those tests include:
4Kscore blood test is a molecular test that helps predict the likelihood and risk of a patient having aggressive prostate cancer. If you’re a patient whose PSA values are borderline for a prostate biopsy or you have a condition that could be aggravated by a biopsy, your physician may use this test before to help determine whether you should get a biopsy or a repeat biopsy.
Urine sample testlooks for biomarkers that may indicate the presence of prostate cancer cells in a patient’s body. This test may also be helpful when trying to determine whether a patient should be rebiopsied or not.
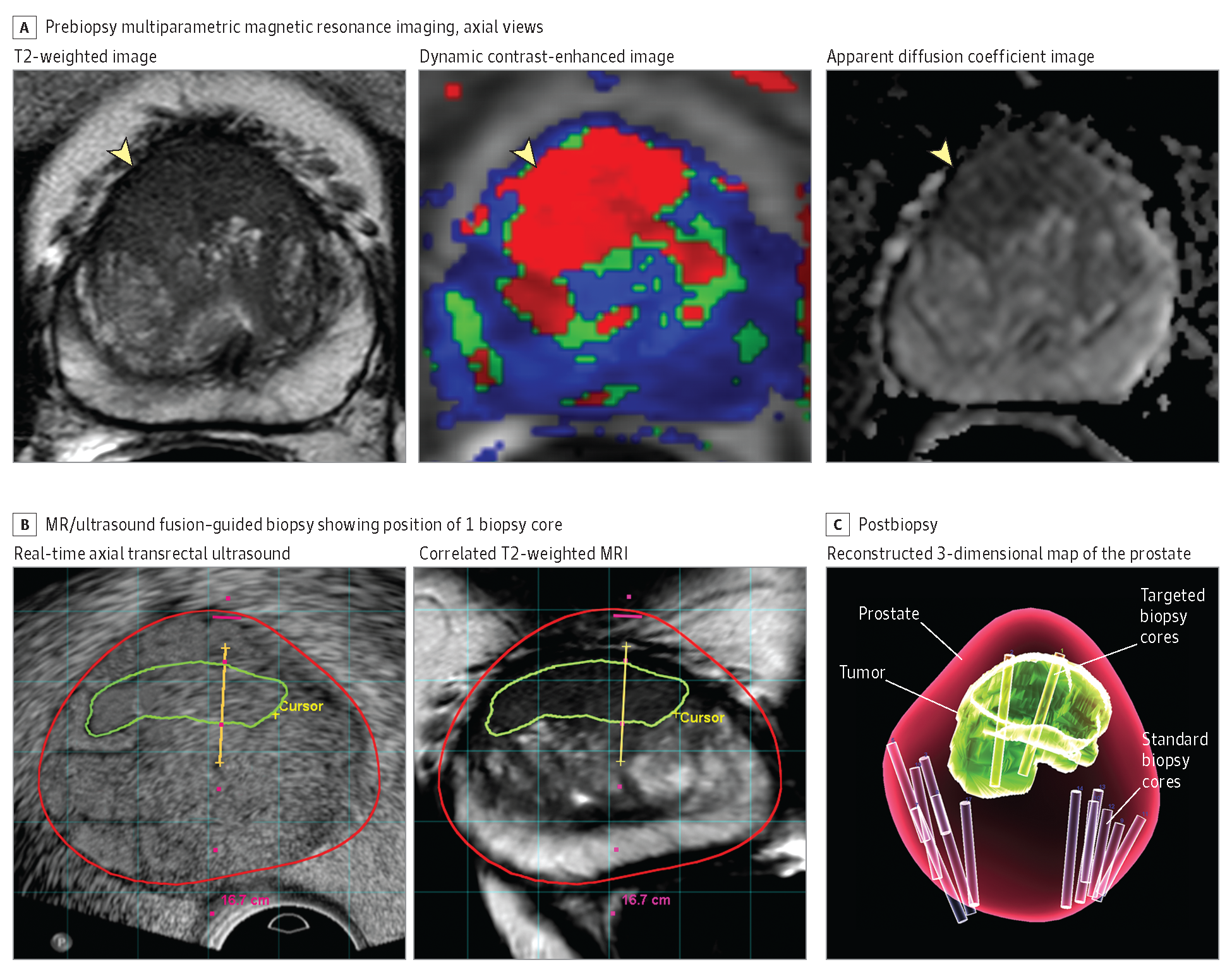
Multiparametric MRI
The use of multiparametric MRI imaging of the prostate gland before a biopsy has been a game changer in prostate cancer diagnosis, increasing the accuracy of biopsies over standard biopsies. The mpMRI doesn’t replace the standard biopsy, but by improving its accuracy, it may help decrease the number of biopsies needed.
The mpMRI has a higher resolution than a standard prostate ultrasound. This increases the ability to see suspicious lesions in the prostate, providing additional targets for the biopsy to sample.
What Are The Benefits Of A Fusion Biopsy
- Fusion biopsy gives a clear view of the locations that need to be sampled. Dr. B-T can guide the needles precisely to those areas.
- Its 30%1 more likely to detect aggressive cancer than a conventional biopsy.
- The prostate MRI is better at distinguishing between tumors that need to be treated and those that arent worrisome. Its 85% effective at finding intermediate or high-grade cancers.
- It can reduce the need for later biopsies by giving better information the first time. A more accurate diagnosis helps to clarify the best treatment course.
Read Also: What Is The Best Over The Counter Prostate Supplement
Lymph Node Biopsy As A Separate Procedure
A lymph node biopsy is rarely done as a separate procedure. Its sometimes used when a radical prostatectomy isnt planned , but when its still important to know if the lymph nodes contain cancer.
Most often, this is done as a needle biopsy. To do this, the doctor uses an image to guide a long, hollow needle through the skin in the lower abdomen and into an enlarged node. The skin is numbed with local anesthesia before the needle is inserted to take a small tissue sample. The sample is then sent to the lab and looked at for cancer cells.
What Are The Side Effects Of A Biopsy
Having a biopsy can cause side effects. These will affect each man differently, and you may not get all of the possible side effects.
Pain or discomfort
Some men feel pain or discomfort in their back passage for a few days after a TRUS biopsy. Others feel a dull ache along the underside of their penis or lower abdomen . If you have a transperineal biopsy, you may get some bruising and discomfort in the area where the needle went in for a few days afterwards.
If you receive anal sex, wait about two weeks, or until any pain or discomfort from your biopsy has settled, before having sex again. Ask your doctor or nurse at the hospital for further advice.
Some men find the biopsy painful, but others have only slight discomfort. Your nurse or doctor may suggest taking mild pain-relieving drugs, such as paracetamol, to help with any pain.
If you have any pain or discomfort that doesnt go away, talk to your nurse or doctor.
Short-term bleeding
Its normal to see a small amount of blood in your urine or bowel movements for about two weeks. You may also notice blood in your semen for a couple of months it might look red or dark brown. This is normal and should get better by itself. If it takes longer to clear up, or gets worse, you should see a doctor straight away.
Infection
Symptoms of a urine infection may include:
- pain or a burning feeling when you urinate
- dark or cloudy urine with a strong smell
- needing to urinate more often than usual
- pain in your lower abdomen .
Also Check: Aggressive Prostate Cancer Survivor Stories
What Will I Experience During And After The Biopsy
If you receive IV contrast for the MRI-guided procedure, you may feel coolness and a flushing sensation for a minute or two following the injection. The IV needle may cause some discomfort when the doctor inserts it and you may have some bruising when they remove it.
Rarely, patients may experience side effects from MR contrast material, such as nausea and local pain, hives, itchy eyes, or other reactions. If you have allergic symptoms, a radiologist or other doctor will be available for immediate assistance.
When the doctor inserts the ultrasound probe or endorectal coil into the rectum, you will feel pressure and may have some temporary discomfort.
You will hear a clicking noise when the biopsy needle samples the prostate and you may feel a stinging or burning sensation in the area.
Some patients find it uncomfortable to remain still during an MRI. Others experience a sense of being closed-in . Sedation is available for patients who anticipate anxiety.
If you feel heating on your skin at any time during MR imaging, tell the MR technician so they can closely examine the area.
Some patients experience a small amount of bleeding from the rectum or perineum immediately after the biopsy. If this does occur, it will cease with gentle pressure.
If you did not receive sedation, no recovery period is necessary. Light general anesthetic or sedation may leave you feeling groggy for a day or so.
Why Choose Loyola For Prostate Fusion Biopsy
Loyola is one of the only centers in the region with the clinical expertise and experience to perform robotic prostate cancer care. Our fellowship-trained cancer surgeons specialize in the biopsy, diagnosis and surgical removal of many types of cancer, working closely with doctors in medical oncology, pathology and radiation therapy. The interdisciplinary team at the MRI/Ultrasound fusion biopsy program provides your patients the best possible cancer care.
Don’t Miss: Stage 4 Prostate Cancer Survival Rate
What To Expect With Mpmri/trus Prostate Fusion Biopsy
UroNav® fusion biopsy is an option for patients with suspected prostate cancer, or for those who have received a negative biopsy for this condition in the past.
This procedure is made up of two parts, a diagnostic prostate MRI and an ultrasound-guided biopsy. The patient first undergoes a prostate MRI which is interpreted by expert radiologists which special training. On a separate visit, the patient undergoes the fusion biopsy as an outpatient by a trained urologist.
Comparison Of Mri/us Fusion
Emerging evidence has shown that multiparametric magnetic resonance imaging as an innovative guidance approach for prostate biopsy increases the detection rate of prostate cancer. Hence, we also reviewed RCT studies comparing MRI/US fusion-guided biopsy and traditional systematic transrectal biopsy. This review was not included in our meta-analysis as our aim was to assess the diagnosis accuracy of transperineal and transrectal biopsy.
In the other RCT study by Kasivisvanathan et al. , the authors randomized 252 patients in an MRI-targeted group and 248 patients in a standard biopsy group. In the MRI-targeted group, 71 patients did not undergo prostate biopsy because of negative MRI results. The patients in the MRI-targeted group received a 4-core MRI/US fusion biopsy and the patients in the standard biopsy group received a systematic transrectal biopsy. Clinically significant prostate cancer was diagnosed in 38% patients in the MRI-targeted group and 26% patients in the standard biopsy group. The detection rate of the MRI-targeted biopsy is significantly higher than the traditional biopsy.
Don’t Miss: Walmart Super Beta Prostate Price
Precancerous Cells And Pin
Sometimes, the results will show that precancerous cells, or prostatic intraepithelial neoplasia , are present.
If these PIN are low grade, the doctor will not consider this a matter of concern. Many males have low grade PIN. However, if the PIN are high grade, there is a chance that cancer may develop. In these cases, a doctor may suggest further tests.
If a person already has prostate cancer, the grade of the PIN does not matter, as it does not affect the severity or the Gleason score of the cancer.
Carcinoma in situ refers to cells that have the potential to become cancerous. They can occur almost anywhere in the body.
What To Expect During An Mri Fusion Biopsy For Elevated Psa
Finding out that your PSA level is high can certainly be unnerving. While the majority of PSA elevations are caused by a benign condition, it’s important to seek further evaluation in order to rule out the presence of prostate cancer. The expert team at Kasraeian Urology, led by renowned board-certified urologists Dr. Ahmad Kasraeian and Dr. Ali Kasraeian, offers advanced diagnostic testing and treatment options for a wide array of urologic conditions in Jacksonville, FL. Learn more about one of the most cutting-edge diagnostic tools for prostate cancer, MRI fusion biopsy, including how it works and what you can expect during the procedure.
Read Also: Is There A Blood Test For Prostate
How Does The Procedure Work
Ultrasound procedure:
Ultrasound imaging uses the same principles as the sonar that bats, ships, and fishermen use. When a sound wave strikes an object, it bounces back or echoes. By measuring these echo waves, it is possible to determine how far away the object is as well as its size, shape, and consistency. This includes whether the object is solid or filled with fluid.
Doctors use ultrasound to detect changes in the appearance of organs, tissues, and vessels and to detect abnormal masses, such as tumors.
In an ultrasound exam, a transducer both sends the sound waves and records the echoing waves. When the transducer is pressed against the skin, it sends small pulses of inaudible, high-frequency sound waves into the body. As the sound waves bounce off internal organs, fluids and tissues, the sensitive receiver in the transducer records tiny changes in the sound’s pitch and direction. A computer instantly measures these signature waves and displays them as real-time pictures on a monitor. The technologist typically captures one or more frames of the moving pictures as still images. They may also save short video loops of the images.
MRI procedure:
A computer processes the signals and creates a series of images, each of which shows a thin slice of the body. The radiologist can study these images from different angles.
MRI is often able to tell the difference between diseased tissue and normal tissue better than x-ray, CT, and ultrasound.