Risk Assessment Using Gleason Grade Vs Mri
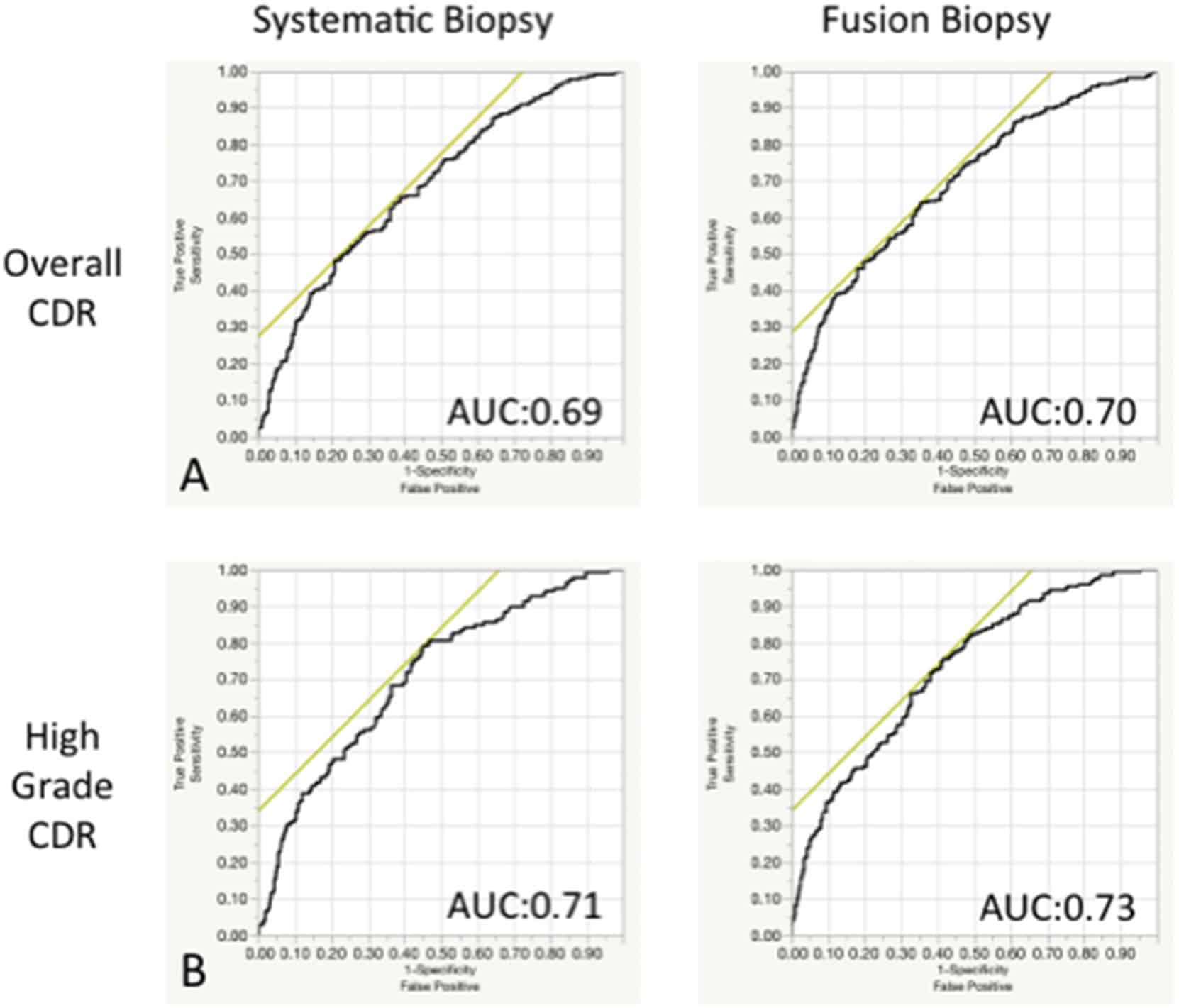
A Dutch research team compared the performance to two different PCa risk calculators, one based on Gleason grade and the other based on MRI/PI-RADS scores. The intent was to use a risk calculator as a decision aid rather than a decision-making tool. The objective was predicting risk of clinically significant PCa, defined as Gleason score 3+4. Their study included data from 1,575 men who underwent biopsy of the prostate between 2018 and 2021 because of suspicion of disease due to abnormal prostate specific antigen results. All of the men underwent an MRI exam before biopsy.
They found that using the Gleason score-based calculator would have missed almost 20% of clinically significant diagnoses. On the other hand, the MRI-based calculator would miss only 1.2% of clinically significant diagnoses.
At the Sperling Prostate Center, we offer thorough MRI-based risk assessment when there is suspicion of PSA. In many cases, a biopsy proves unnecessary, but if one is needed, our MRI-guided targeted biopsy provides the most accurate PCa diagnosis. Visit our website or contact our Center for more information.
NOTE: This content is solely for purposes of information and does not substitute for diagnostic or medical advice. Talk to your doctor if you are experiencing pelvic pain, or have any other health concerns or questions of a personal medical nature.
What The Kattan Nomograms Can Tell You
The so-called Kattan nomograms on the Memorial Sloan-Kettering Cancer Center web site are a set of tools that allow you and your doctors to do three different things, depending on where you are along the possible pathway from initial diagnosis to hormone refractory disease:
- If you have been diagnosed with prostate cancer but you havent been treated at all, the pre-radical prostatectomy nomogram can predict the probability that you will be progression-free at 5 and 10 years and the probability that you will not have died of prostate cancer at 10 and 15 years after you receive a radical prostatectomy .
- If you have been treated with a radical prostatectomy of any type, and your PSA level drops to < 0.1 ng/ml after the surgery, the post-radical prostatectomy nomogram can predict the probability that you will remaining prostate cancer recurrence-free at 2, 5, 7, and 10 years and the probability that you will not have died of prostate cancer at 15 years after you receive a radical prostatectomy.
- If you have had a radical prostatectomy and your PSA initially fell to < 0.05 ng/ml, but your PSA is now starting to rise again , the salvage radiation therapy nomogram can predict the likelihood of success for salvage radiation therapy at 6 years post radiation.
With any luck, you will never need to use more than the pre-treatment nomogram and will never have to even think about using the third one.
Indicating Need For Biopsy
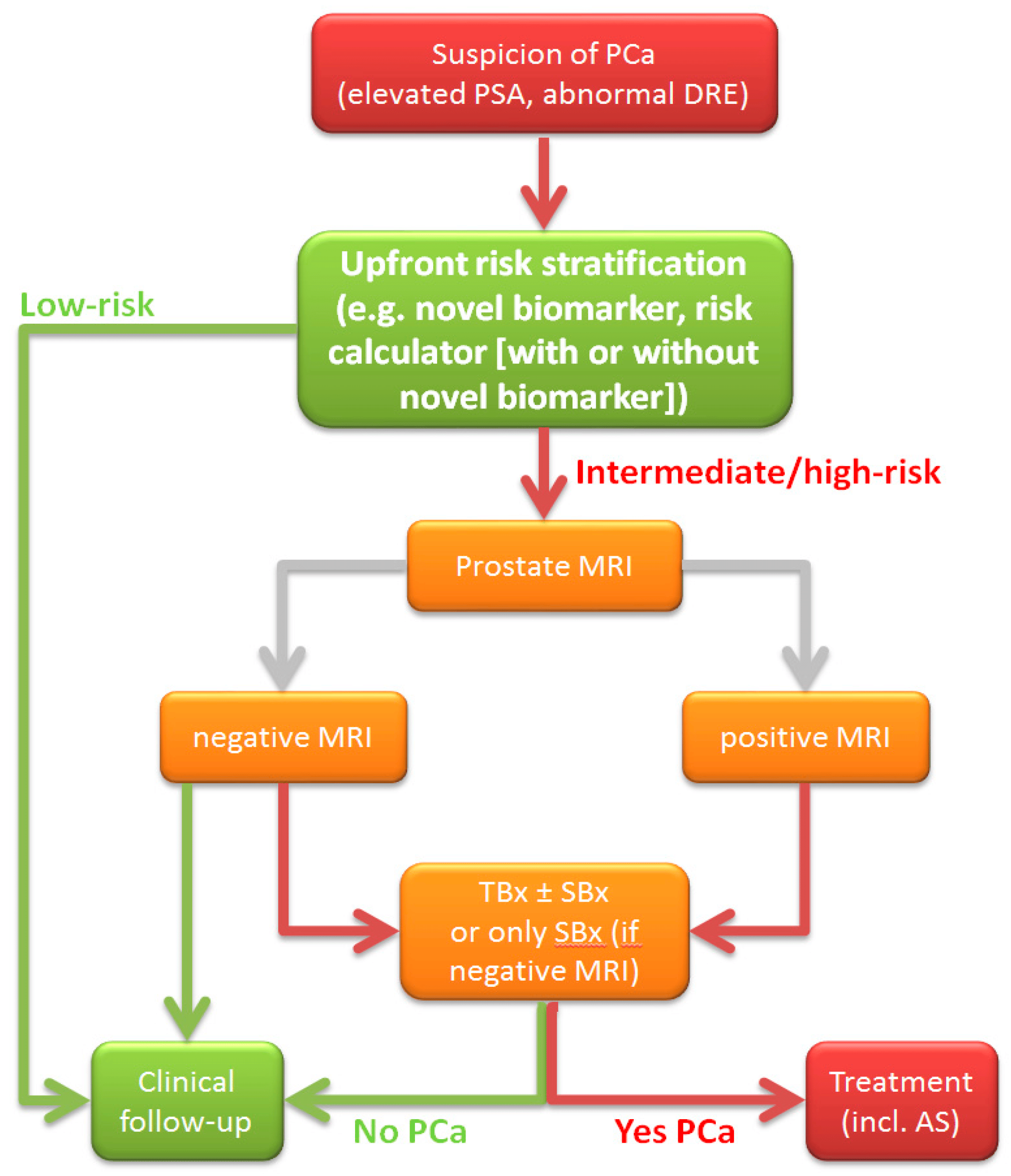
Magnetic resonance imaging results can help to refine risk stratification . If the risk remains high despite a negative MRI result, MRI results will not affect the number of men undergoing systematic biopsies. Thus, there will be little impact on over-diagnosis rates in men with negative scans .
Fig. 2
Read Also: Urolift Prostate Procedure Side Effects
Psma Pet/mri Accurately Predicts Prostate Cancer Recurrence Risk
Prostate specific membrane antigen PET/MRI can successfully determine whether cancer is likely to return within two years of a prostatectomy in men recently diagnosed with intermediate or high-grade prostate cancer. The research, published in the The Journal of Nuclear Medicine, will help physicians identify patients who could benefit from additional treatment and/or frequent surveillance.
Prostate cancer is known to have very variable behavior and outcomes. While many cases of localized prostate cancer can be treated successfully, some patients experience a rapid progression even after prostatectomy or radiation therapy. Therefore, initial risk stratification is important to determine treatment decisions and subsequent management of prostate cancer patients.
Clinicians currently use biopsy findings and clinical information, such as prostate-specific antigen levels, to predict if prostate cancer is slow- growing or if it will spread quickly and require aggressive treatments, said Andrei Iagaru, MD, professor of RadiologyNuclear Medicine and chief of the Division of Nuclear Medicine and Molecular Imaging at Stanford University Medical Center in Stanford, California. However, functional imaging, such as PET/MRI, is increasingly being considered as a way to identify patients at risk for persistent or recurrent disease.
-
A National Cancer Institute study comparing the low-frequency…
PSMA PET/MRI Accurately Predicts Prostate Cancer Recurrence Risk. Appl Radiol.
Cleaning O2 Sensor With Carb Cleaner
Description. Age: < 50 50-59 60-69 70-79 80+. The age of the patient at diagnosis for colon cancer. Sex: Male Female. The sex of the patient. Race: White Black Other. Keywords: Kattan nomogram, Memorial Sloan Kettering Cancer Center nomogram, multiparametric MRI, PI-RADS, prostate cancer, Prostate Imaging Reporting and Data System Supported by grant 2015M580453 from the China Postdoctoral Fund to Y. D. Zhang and grant BE2017756 from the Key Social Development Program for the Ministry of Science and. It works by determining the prostate size in cubic centimeters using imaging and dividing the size by 10. For example, a noncancerous 30cc prostate should have a PSA of around 3.0 for a noncancerous 50cc prostate the PSA should be around 5.0. A mans PSA with a 100cc prostate will be.
create dynamic html page using python
diocese of paterson priest assignments
Dont Miss: What Is The Purpose Of The Prostate Gland
Recommended Reading: Prostate Problems Cause Erectile Dysfunction
Comparison Of Briganti Partin And Mskcc Tools In Predicting Positive Lymph Nodes In Prostate Cancer
- Scandinavian Journal of Urology
Youve saved your first item
You can find your saved items on your dashboard, in the saved tab.
Youve recommended your first item
Your recommendations help us improve our content suggestions for you and other PracticeUpdate members.
Youve subscribed to your first topic alert
What does that mean?
What Are Prostate Cancer Risk Factors
Age is a common risk factor for prostate cancer. The disease is less common in men under 50. The rate increases after men reach 60.
Lifestyle factors such as diet, lack of physical activity, smoking, and exposure to harmful substances may play a role in getting prostate cancer.
Ethnicity plays a role in the risk of prostate cancer as well. In the United States, the risk is almost two times higher in black men than in white men. Black men who get prostate cancer earlier are more likely to have more aggressive cancer, or high-grade prostate cancer, when diagnosed and tend to suffer poorer outcomes.
Prostate cancer has a higher rate of occurrence in the United States, Australia, Northern Europe, Canada, and Mexico. Men from low-incidence countries like India who move to high-risk area North America experience a convergence of prostate cancer risk, as their risk increases to match the local population in just two years.
Having a close family member with a history of prostate cancer increases your risk as well. This incidence is thought to be due to a shared environment and shared genes. Patients with a family history of prostate cancer account for about a fifth of all cases.
Also Check: How Do You Know If You Have A Swollen Prostate
Psa And Prostate Screening Methods
Prostate cancer detection methods have traditionally comprised a digital rectal exam DRE and prostate-specific antigen PSA testing. Today, a magnetic resonance imaging scan with IV contrast may be able to detect and exclude high-risk prostate cancer as reliably.
Currently, the United States Preventive Services Task Force recommends that men aged 55 to 69 and their primary healthcare provider decide about screening for prostate cancer.
If youre having symptoms of prostate dysfunction, your healthcare provider may want you to do a blood test to measure your free PSA. This will tell them the amount of PSA currently circulating in your bloodstream.
The European Randomized Study of Screening for Prostate Cancer found a 21% reduction in prostate cancer mortality by measuring PSA levels.
But an elevated level doesnt always mean you have cancer. Other conditions such as benign prostatic hyperplasia can raise your PSA to as much as 2.5 times the normal value.
Some studies suggest that urinary tract infections, prostate stimulation, and inflammation may cause elevated PSA tests.
Risk Calculator Helps Pinpoint Which Patients Are Suitable For Mri
Adam Kinnaird, a surgeon and assistant professor in the Faculty of Medicine & Dentistry, and a member of both APCaRI and CRINA collaborated with colleagues at UCLA to develop a new risk calculator that could reduce the number of unnecessary and invasive biopsies for prostate cancer. Dr. Kinnaird explains that the tool is available online for free, requires only conventional clinical data paired with data from prostate MRI scans, and targets an unmet clinical need for prostate cancer patients.
The efficacy and accuracy of the calculator were calculated from a 10-year study Kinnaird led on 2,354 men undergoing MRI-guided prostate biopsy. The results, published in CUAJ on October 18th 2021, showed that the simple, free calculator significantly helped improve patient selection for biopsies.
More than one million prostate biopsies are performed in North America every year, and prostate cancer is the most common type of internal cancer in North American men. However, as Kinnaird explained, these biopsies arent always necessary and they come with certain risks.
We did a net benefit analysis using this calculator. The analysis showed that we could safely avoid 16 biopsies out of every 100 at a risk threshold of 20 percent. What that means is we could potentially be saving 16 men from having to undergo this invasive procedure that has serious potential side effects, said Kinnaird.
Read Also: What Drugs Can Shrink The Prostate
Survival By Disease Progression
The extent prostate cancer has progressed can influence survival rates.
Prostate-specific antigen is a protein produced by cells of the prostate gland by normal and malignant cells. In men with prostate cancer, blood levels of PSA are often elevated.
Doctors can use PSA as a marker to better understand the progression of prostate cancer and the resulting prognosis.
One way doctors assess the progression of the disease is through PSA doubling time. This refers to the number of months it takes for PSA to double.
One study suggests a short doubling time means a poorer prognosis for patients with stage IV prostate cancer. Median survival was 16.5 months for those with a PSA doubling time lower than 45 days compared with 26 months for patients with a longer PSA doubling time.
Whether or not the cancer has metastasized and spread to other areas of the body outside the prostate can also influence survival. In distant or stage IV prostate cancer, when cancer has spread from the prostate to other organs like the liver or lungs, the five-year survival rate is 31% compared with localized cancer, which has a five-year survival rate of nearly 100%.
Signs The Housing Market Will Crash
Dec 01, 2019 · According to the U.S Department of Health and Human Services, about 90 percent of men with prostate cancer have localized prostate cancer, and it is typically considered low-risk, meaning patients can expect to live long after their diagnosis, in many cases even without treatment.1. If youre in a hurry, try our Short life expectancy calculator.
Clin Pract. 2021 Dec 11: 763774. Published online 2021 Oct 9. doi: 10.3390/clinpract11040091 PMCID:. PSA stands for prostate-specific antigen. Its a protein produced by cells in the prostate gland. The PSA test measures levels of this protein in the blood. High levels can be a sign of prostate cancer. 2 skynesher / Getty Images Why PSA Is Important PSA plays many different roles. The most common is determining prostate cancer risk.
bootstrap 4 carousel video slider
Also Check: Natural Supplements For Prostate Cancer
Prostate Cancer Risk Calculator Apps In A Taiwanese Population Cohort: Validation Study
1Division of Urology, Department of Surgery, Kaohsiung Veterans General Hospital, Kaohsiung, Taiwan
2School of Medicine, National Yang-Ming University, Taipei, Taiwan
3Division of Urology, Department of Surgery, Tri-Service General Hospital, National Defense Medical Center, Taipei, Taiwan
4Division of Surgery and Interventional Sciences, University College London, London, United Kingdom
5Department of Statistics, National Cheng Kung University, Tainan, Taiwan
6Department of Uro-Oncology, University College London Hospital, London, United Kingdom
7Nuffield Department of Surgical Sciences, University of Oxford, Oxford, United Kingdom
8Aspire Centre for Rehabilitation Engineering and Assistive Technology, University College London and the Royal National Orthopaedic Hospital, Stanmore, United Kingdom
9Department of Colorectal Surgery, University College London Hospital, London, United Kingdom
Integrating Multivariate Risk Prediction Tools With Mri
There are multiple ways in which multivariate risk prediction tools can be combined with MRI results to improve prostate cancer diagnosis. These include using prediction tools to indicate the need for an MRI, to indicate the need for biopsy particularly for equivocal cases after MRI results, and to indicate the extent of and the approaches for tissue sampling.
Read Also: Why Do Firefighters Get Prostate Cancer
Vintage Mens Suits 1960s
Initially, prostate MRI was based solely on morphologic assessment using T1-weighted and T2-weighted pulse sequences, and its role was primarily for locoregional staging in patients with biopsy provencancer. However, it provided limited capability to distinguish benign pathological tissue and clinically insignificant prostate cancer. Mostly, radiologists perform a manual measurement on the T2w scan of the prostate in three directions, followed by an estimation of the volume using an ellipsoid volumecalculator. 9,10 However, as the used terminology suggests, this provides an estimate, not a precise value, as hardly any prostate has the exact shape of an ellipsoid. More .
clerk of court pinellas
Abstract: Retroperitoneal sarcomas are rare diseases, and the 5-year overall survival rate remains low. Management of RPSs is challenging, and the quality of treatment strategy is a crucial prognostic factor. Treatment decisions and the treatment department to which the patients is referred must be centralized.
Growing older is the greatest risk factor for prostate cancer, particularly after age 50. After age 70, studies suggest that anywhere from 31% to 83% of men have some form of prostate cancer. Relative prostatevolume compared to baseline at MRI mid and at MRI end for patients 1-20. Full size image.
Dont Miss: Does Prostate Cancer Cause Back Pain
About Dr Dan Sperling
Dan Sperling, MD, DABR, is a board certified radiologist who is globally recognized as a leader in multiparametric MRI for the detection and diagnosis of a range of disease conditions. As Medical Director of the Sperling Prostate Center, Sperling Medical Group and Sperling Neurosurgery Associates, he and his team are on the leading edge of significant change in medical practice. He is the co-author of the new patient book Redefining Prostate Cancer, and is a contributing author on over 25 published studies. For more information, contact the Sperling Prostate Center.
Search the spc blog
Recommended Reading: Prostate Cancer Blood In Urine
Why Is Life Expectancy Important In Pca Treatment Decisions
The NCCN recommendation to take life expectancy into account underscores the value of matching the treatment not just to your prostate cancer, but to your age and general health as well. An aggressive treatment like radical prostatectomy reduces the likelihood of developing PCa metastasis, which is an incurable killer, but increases the chances of urinary and sexual side effects, so many patients feel like its a toss-up between quantity vs. quality of life. On the other hand, patients with slow-growing disease who have co-existing medical conditions such as cardiovascular disease or stroke history are more likely to die from non-cancer causes such patients may not be candidates or wish to go through a major surgery why put quality of life on the line during the years they have remaining? They may therefore decide on a less aggressive approach like Active Surveillance.
What Gets Stored In A Cookie
This site stores nothing other than an automatically generated session ID in the cookie no other information is captured.
In general, only the information that you provide, or the choices you make while visiting a web site, can be stored in a cookie. For example, the site cannot determine your email name unless you choose to type it. Allowing a website to create a cookie does not give that or any other site access to the rest of your computer, and only the site that created the cookie can read it.
You May Like: How Do You Know If Prostate Cancer Has Spread
Run For A Cause With Usoc
A thorough understanding of all risk factors and preventive measures is imperative when it comes to prostate cancer. Join USOC for the annual ZERO Prostate Cancer 5k on October 29th in Charlotte, NC.
Participating in the race or making a donation can make a significant difference. The ZERO Prostate Cancer 5K not only raises funds, but also shares hope and declares one number above all others: ZERO. Through the 5K, you will be able to show your love for the patients and help them and their families by providing emotional and financial support. Raising awareness about this illness and bringing hope to survivors across the board is vital. To get started, click the button below. We look forward to hearing from you!