Faq: Radiation Therapy For Prostate Cancer
Why would I choose radiation therapy?
Radiation therapy, including external beam radiation therapy and brachytherapy, is an alternative form of treatment for prostate cancer. EBRT may be used after other treatments, such as surgery, to manage cancer that has recurred or is at high risk of recurrence. Radiation therapy has an excellent record of success, providing long-term disease control and survival rates equivalent to other treatments, including surgery.
How should I expect to feel during radiation therapy?
Undergoing external beam radiation therapy is similar to having a routine X-ray. Radiation cannot be seen, smelled or felt. Generally, side effects don’t appear until the second or third week of treatment. Because radiation therapy is a local treatment, only the areas of the body where it is directed will experience side effects. Most patients will experience some or all of the following:
- Increase in the frequency of urination
- Urinary urgency
- Softer and smaller volume bowel movements
- Increased frequency of bowel movements
- Worsening of hemorrhoids or rectal irritation with occasional scant blood and fatigue
Many questions may arise during radiation therapy treatment. Your doctors will be available to answer questions throughout your treatment.
How should I expect to feel after radiation therapy?
What Are The Side Effects Of Brachytherapy
- Frequent urination or urinary retention or burning with urination
- Erectile dysfunction
- Urethral stricture or narrowing of the urethra
- Diarrhea or blood in the stool
- Secondary cancers
For the short time that the seeds are giving off larger amounts of radiation, you should avoid close proximity to children or pregnant women. Make sure to talk with your radiation oncologist or oncology nurse for instruction about radiation safety and exposure for family members or pets.
If you are traveling through an airport following brachytherapy treatment, there is a chance that radiation detectors will be set off. Talk to your radiation oncologist and ask for a note to indicate youve just had radiation treatment.
Whats It Like To Have External Beam Radiation Therapy For Prostate Cancer
Before you undergo external beam radiation therapy, your clinical team will map out where the cancer is located so that they can better target the radiation therapy. The goal is to treat just that area, and nothing more. This will reduce your chances of experiencing side effects. This process typically includes:
- A radiation simulation where the clinical team helps you find the most comfortable spot to rest in during your treatment
- Computerized tomography scanning so that your doctors can precisely map the area of your body that needs treatment
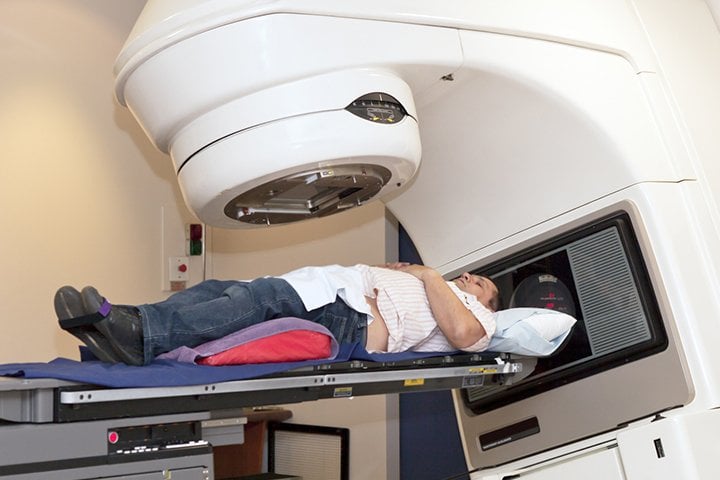
During the external beam radiation treatment, you will rest on a table and hold very still while the linear accelerator moves around you to deliver the treatment. You may have an immobilization device to hold you in position to ensure the radiation goes exactly where it should. Your job during the treatment is to relax, breathe normally, and hold still. External beam radiation therapy for your prostate is not a painful treatment. You should be able to rest comfortably while the treatment is given.
The machine will deliver a very precise dose of radiation prescribed by your doctor. Each treatment usually lasts less than an hour and most of that time is spent preparing for the dosage. The radiation treatment itself is usually just a few minutes. During this time, your clinical team will be outside the room but able to see and talk with you through cameras and an audio connection.
Don’t Miss: What Is Super Beta Prostate
What Types Of Radiotherapy Are There
There are two common types of external beam radiotherapy:
- intensity-modulated radiotherapy
- 3-dimensional conformal radiotherapy .
You may also hear about image guided radiotherapy . This is part of all radiotherapy treatments. Taking images of the prostate before each treatment allows your radiographer to make small changes to the area that is going to be treated, in case the prostate has moved slightly since your last treatment session. This makes sure the surrounding healthy tissue gets as little radiation as possible. It also makes sure the whole prostate is treated.
Intensity-modulated radiotherapy
This is the most common type of external beam radiotherapy in the UK. A computer uses the scans from your radiotherapy planning session to map the location, size and shape of your prostate. The radiotherapy machine gives beams of radiation that match the shape of the prostate as closely as possible. This helps to avoid damaging the healthy tissue around it, reducing the risk of side effects.
The strength of the radiation can be controlled so that different areas get a different dose. This means a higher dose of radiation can be given to the prostate without causing too much damage to surrounding tissue.
3D conformal radiotherapy
As with IMRT, the radiation beams are mapped to the size, shape and position of the prostate. But the strength of the radiation cant be controlled in 3D-CRT, so all areas are treated with the same dose.
Other types of radiotherapy
Proton beam therapy
Ebrt After Radical Prostatectomy
Radiation therapy has been used as an adjuvant after surgical treatment of prostate cancer . Selection of candidates for this approach is increasingly difficult. Prognostic variables that predict extracapsular extension can be used before the selection of surgical candidates. Unfortunately, many of the clinical trials that attempted to answer the role of postsurgical radiotherapy were conducted before the era of PSA testing.
Multi-institutional data from the American Society of Therapeutic Radiation Oncology consensus conference suggest that in patients treated for a rising PSA level, postoperative radiotherapy offers a PSA remission rate of 70%. Unfortunately, the durability of this response varies widely from center to center, with averages ranging from 25 to 67 months. The ASTRO panel also noted that the data support initiation of therapy when the PSA level is below 1.5 ng/mL.
Subsequently reported data further support the use of adjuvant radiotherapy, indicating improved biochemical control of disease with immediate postoperative therapy as compared with benefits seen when treatment is started for a rising PSA level. Finally, the ASTRO panel noted that the use of hormonal therapy in this setting is investigational.
Don’t Miss: Steps To Prevent Prostate Cancer
How Does External Beam Radiation Therapy For Prostate Cancer Work
Nearly 250,000 men will be diagnosed with prostate cancer this year. Prostate cancer is second only to skin cancer as the most common type of malignant cancer that men experience. While prostate cancer is a terrible diagnosis for you to hear, there is hope in the fact that the 10-year survival rate for this disease is 98%.
The death rate from prostate cancer has been dropping steadily thanks to earlier diagnosis of the disease and the new technologies that improve treatment for it. This article discusses one of the most innovative treatment approaches available today to men with prostate cancer: external beam radiation therapy.
Do We Know Which Treatment Is Better For Prostate Cancer Brachytherapy Or External Beam Radiation
Its not a question of which therapy is better but rather which therapy is the most tailored, pinpointed radiation for the patients specific disease.
When it comes to early stages of disease, patients very frequently do well with either brachytherapy or external beam radiation. Success rates of around 90% or higher can be achieved with either approach. When the disease is somewhat more advanced based on the PSA level or the Gleason score or visible evidence of disease on an MRI we have learned over the years that higher doses of radiation are critical to achieving better results. Some evidence suggests that for patients with intermediate- or high-risk prostate cancer, a combined approach using brachytherapy along with external beam radiation may be best.
Data that we have published recently show that for patients with intermediate-risk disease, the combination of external beam radiation with brachytherapy not only provides better biochemical control, in terms of PSA level, but also reduces the risk of distant metastases, or spread of the disease. Another recent study from Canada, which compared outcomes in patients who were treated with external beam radiation or a combination approach, found superior results when the combined approach was used. These studies provide strong evidence that higher doses of radiation provide an important benefit to patients with intermediate-risk and high-risk prostate cancers.
Also Check: My Husband Has Prostate Cancer
Possible Side Effects Of Radiation Treatment For Prostate Cancer
The radiation used to destroy cancer cells can also hurt normal cells in the nearby area. Side effects from radiation treatment are related to the area of the body being treated. Patients start to have side effects a few weeks into their treatment. While side effects may be unpleasant, there are treatments to help deal with them. Most side effects are temporary and slowly start to go away once treatment is done.
You will be seen by your radiation oncology providers often during treatment. These visits are a chance to ask questions and to talk about any side effects and how to best manage them. You can also call your providers to speak about any side effects.
What Is Stereotactic Body Radiation Therapy And What Advantages Does It Offer
Traditionally, we deliver external beam radiation in 45 to 48 sessions over a span of ten weeks, using very sophisticated computer-based planning and enhanced imaging techniques and tumor tracking during the treatment. This is called image-guided IMRT and it is the current standard of care.
But there is increasing interest in giving this radiation in shorter courses of treatment. Many of the people we care for have a type of radiation therapy called MSK PreciseTM. MSK Precise is a form of SBRT that can be given in five sessions instead of the usual 45 to 50. MSK has been doing this for the past nine years, and the results in the several hundred people whove been treated have been excellent so far. The treatment is very well tolerated, with outcomes that are at least equivalent to and possibly better than the standard ten weeks of treatment. Because of its superior precision, MSK Precise has less side effects than more conventional radiation techniques, with extremely low rates of incontinence and rectal problems. The sexual side effects are low and similar to what is experienced with conventional external radiation techniques. And of course, its much more convenient for patients.
For patients with more-advanced tumors, we are completing a phase II trial in which were combining sophisticated brachytherapy approaches with MSK Precise. This kind of combination of dose-intense or escalated radiation may end up being a very effective regimen.
Also Check: Enlarged Prostate Blood In Urine
What Happens During A Treatment Session
- You may be asked to change into a hospital gown or robe.
- You will go to the treatment room where you will receive radiation. The temperature in this room will be very cool.
- Depending on where your cancer is, you will either lie down on a treatment table or sit in a special chair. The radiation therapist will use the dots on your skin and body mold or face mask, if you have one, to help place you in the right position.
- You may see colored lights pointed at your skin marks. These lights are harmless and help the therapist position you for treatment.
- You will need to stay very still so the radiation goes to the exact same place each time. You will get radiation for 1 to 5 minutes. During this time, you can breathe normally.
The radiation therapist will leave the room just before your treatment begins. He or she will go to a nearby room to control the radiation machine. The therapist watches you on a TV screen or through a window and talks with you through a speaker in the treatment room. Make sure to tell the therapist if you feel sick or are uncomfortable. He or she can stop the radiation machine at any time. You will hear the radiation machine and see it moving around, but you won’t be able to feel, hear, see, or smell the radiation.
Most visits last from 30 minutes to an hour, with most of that time spent placing you in the correct position.
Next Steps & Resources:
- Learn more about our featured clinical experts:
- Glen Gejerman, M.D., co-director of urologic oncology at Hackensack Meridian Healths John Theurer Cancer Center and associate professor of Oncology at the Hackensack Meridian School of Medicine.
- Prashant Desai, M.D., medical director of radiation oncology at Hackensack Meridian Ocean Medical Center.
- Priti Patel, M.D., medical director of radiation oncology at Hackensack Meridian Riverview Medical Center.
- US News & World Report has recognized Hackensack Meridian John Theurer Cancer Center as the best cancer center in New Jersey. To schedule a visit or a second opinion call 551-996-5855.
- We also offer cancer services across Hackensack Meridian Health at several convenient locations near you. To schedule a visit or a second opinion call1-844-HMH-WELL.
Recommended Reading: What Is A Prostate Test
Possible Side Effects Of Ebrt
Some of the side effects from EBRT are the same as those from surgery, while others are different.
Bowel problems: Radiation can irritate the rectum and cause a condition called radiation proctitis. This can lead to diarrhea, sometimes with blood in the stool, and rectal leakage. Most of these problems go away over time, but in rare cases normal bowel function does not return. To help lessen bowel problems, you may be told to follow a special diet during radiation therapy to help limit bowel movement during treatment. Sometimes a balloon-like device or gel is put between the rectum and the prostate before treatment to act like a spacer to lessen the amount of radiation that reaches the rectum.
Urinary problems: Radiation can irritate the bladder and lead to a condition called radiation cystitis. You might need to urinate more often, have a burning sensation while you urinate, and/or find blood in your urine. Urinary problems usually improve over time, but in some men they never go away.
Some men develop urinary incontinence after treatment, which means they cant control their urine or have leakage or dribbling. As described in the surgery section, there are different levels and types of incontinence. Overall, this side effect occurs less often with radiation therapy than after surgery. The risk is low at first, but it goes up each year for several years after treatment.
Who Should Consider External Beam Radiation Therapy

In most cases, external beam radiation therapy is used for men with localized prostate cancer . The intent of EBRT in this case is to kill the tumor while sparing as much healthy tissue as possible. Sometimes it is used in more advanced cases. For example, it can be used along with hormone therapy, or used to relieve pain from bone metastases.
You May Like: Signs Of Prostate Cancer Mayo Clinic
Is There Any Special Preparation Needed For The Procedure
The process of external beam therapy involves three parts:
- Simulation
- Treatment Planning
- Treatment Delivery
The goal of simulation is to determine the treatment position that will be used daily, to make devices that will help the patient maintain that position, and to obtain the necessary images for treatment planning. The radiation therapist places the patient in the treatment position on a CT scanner. Masks, pads or other immobilization devices are typically used to help the patient to hold still and in a specific position during the simulation. These devices will be used for the treatment to achieve the same position daily, so it is important that the patient can maintain that position. Images of the treatment area are taken in the treatment position. The radiation therapist places small marks on the patients to help guide the daily treatments. These marks may be tattoos or colored ink. The tattoos will be permanent, but the colored ink will eventually fade. Marker seeds may be placed in the target tumor or organ at simulation or during a separate surgical procedure. These seeds or markings are intended to help the radiation therapist position the patient during each treatment session.
After the simulation and planning have been completed, the treatment can begin.
How Does Your Doctor Plan Your Radiation Treatment
Radiation is planned and given by a team of trained health care providers. The radiation oncologist is a doctor who treats cancer with radiation and oversees the care of each patient getting radiation. Working closely with the radiation oncologist, the radiation therapist gives the daily radiation treatment and positions patients for each treatment. Other professionals include the medical physicist and dosimetrist who plan and calculate the doses of radiation.
Before starting radiation therapy, your radiation oncologist will examine you, review your medical history and test results, and pinpoint the exact area to be treated. This planning session is called simulation. You might hear this referred to as the sim. Youll be asked to lie still on a table while the radiation therapist uses imaging scans to define your treatment field . These are the exact places on your body where the radiation beams will be aimed.
The simulation is very important and may take some time. Itâs used to plan exactly where the treatment will be on or in your body. The radiation can then be delivered as directly as possible to the tumor while affecting normal, healthy tissues as little as possible.
You May Like: Clinical Synergy Complete Prostate Health
Read Also: What To Eat For Prostate Health
Stereotactic Body Radiation Therapy Or Stereotactic Ablative Radiotherapy
This type of therapy is used to deliver high doses of radiation to a precise area in the prostate using specialized techniques not achievable by standard conventional radiation therapy. This allows the total dose of radiation to be given in a shorter amount of time, usually 4 -5 treatments over 1 2 weeks rather than the several weeks used for other types of external radiation therapy.
The radiation beam needs to be extremely accurate in order to limit the side effects on healthy tissue. During treatment, the body immobilization used is often more restrictive than with IMRT due to the high doses of radiation. Fiducials, or internal prostate markers, are often used in this type of treatment.
Cyberknife and Truebeam are two types of LINACs used for SBRT treatment of prostate cancer.