Why Does It Happen
- At the point where the bladder and urethra join, there is a ring of muscles known as the bladder neck sphincter, which opens and closes like a camera shutter. The bladder neck sphincter is closed most of the time to prevent urine leaking out, but when it gets a signal from the brain, it opens to allow urine to be passed.
- If the bladder neck sphincter is damaged during prostate cancer surgery, this can lead to urinary incontinence.
- Another sphincter is part of another set of muscles below the prostate called the pelvic floor. These muscles are also involved in bladder control.
Most men regain their bladder control over time and are fully recovered within 6 to 12 months. It is important to get professional advice to help cope bladder weakness during this time.
Surgery For Prostate Cancer
Surgery is a common choice to try to cure prostate cancer if it is not thought to have spread outside the prostate gland.
The main type of surgery for prostate cancer is a radical prostatectomy. In this operation, the surgeon removes the entire prostate gland plus some of the tissue around it, including the seminal vesicles.
Open Or Laparoscopic Radical Prostatectomy
In the more traditional approach to prostatectomy, called anopen prostatectomy, the surgeon operates through a single long skin incision to remove the prostate and nearby tissues. This type of surgery is done less often than in the past.
In a laparoscopic prostatectomy, the surgeon makes several smaller incisions and uses special long surgical tools to remove the prostate. The surgeon either holds the tools directly, or uses a control panel to precisely move robotic arms that hold the tools. This approach to prostatectomy has become more common in recent years. If done by experienced surgeons, the laparoscopic radical prostatectomy can give results similar to the open approach.
Don’t Miss: Best Prostate Over The Counter Medicine
Turning Off Your Artificial Urinary Sphincter:
Once your AUS is on, there may be certain times when your AUS should be turned off. Your caregiver will show you how to turn the AUS on and off. You may need to turn off your AUS at the following times:
- At night: Your caregiver may tell you to turn off your AUS each night when you go to bed. Turning off the AUS helps decrease pressure on your urethra and helps prevent damage. You can wear a pad at night to help absorb any urine leakage.
- At the end of a pregnancy: Pregnant women may need to turn off their AUS for the last three months of pregnancy. Turning off the AUS decreases the pressure on the urethra and helps prevent damage. Turning off the AUS also helps prevent AUS cuff damage from the pressure of the unborn baby’s head. Talk with your caregiver if you have any questions or concerns about your AUS and pregnancy.
- For procedures: You may need to turn off your AUS before procedures that involve your urinary tract. These procedures include urinary catheter placement or a cystoscopy . Your caregiver may give you a card to carry that has information about your AUS. Show the card to caregivers to see if your AUS should be turned off during a procedure.
What Types Of Incontinence Can Occur After Radical Prostatectomy Surgery

There are two main types of urinary incontinence in men after radical protatectomy:
- Urgency incontinence
- Stress urinary incontinence
Urgency incontinence is when you feel the “urge” to urinate but cannot make it to the toilet in time. This is generally due to bladder spasms and often responds to medical therapy. This type of incontinence is thought to be mostly due to changes in the way the bladder behaves after surgery.
Stress urinary incontinence , is leakage of urine with exertion or effort and can happen when you cough, sneeze, lift something heavy, change position, swing a golf club or exercise. This type of incontinence may be because of damage to your external sphincter muscle as described above. Almost all men will have some degree of SUI immediately after catheter removal, and you were probably given instructions on how to perform pelvic floor exercises to improve urinary control.
Recommended Reading: Bipolar Androgen Therapy Prostate Cancer
How Is Urinary Incontinence After Prostate Surgery Treated
If you find youre having issues with mild to moderate leakage after surgery, your healthcare provider might suggest starting with noninvasive therapies like medications or physical therapy exercises for the pelvic floor muscles. These treatments may also cut down on the number of times that you have to get up each night to pee.
These methods can sometimes help men who have mild to moderate leakage. Men who have persistent leakage or a more severe problem may need surgery if they do not want to continue to use pads.
When To Exercise The Male Kegal Muscles
* You can perform male Kegel exercises anywhere at any time. People around you will not even know you are doing them. Take advantage of this by incorporating kegel exercises into your daily routine. For example, you can do them while driving a car, waiting in line, watching television, reading a book. Be sure to exercise daily. The more you do, the better. * You can also do these when you have an incontinent episode. For example, if you are experiencing urinary leakage on the way to the bathroom, stop and do a few kegel exercises until the leakage stops and then continue to the bathroom. If you leak urine when you cough, tighten the muscles quickly as you cough to reduce leakage. This is your best method of reducing leakage at inconvenient times.
Recommended Reading: Best Diet To Fight Prostate Cancer
When To Call Your Healthcare Provider
-
Youre not able to urinate, or notice a decrease in urine flow
-
You have a fever of 100.4°F or higher, or as directed by your doctor
-
You have severe pain that is not relieved by prescription pain medicine
-
You have bleeding that doesnt stop within 12 hours
-
You have bleeding with clots, or blood plugs up the catheter.
-
The catheter falls out
Evaluation Of Incontinence After Prostate Treatment
Guideline Statement 9
Clinicians should evaluate patients with incontinence after prostate treatment with history, physical exam, and appropriate diagnostic modalities to categorize type and severity of incontinence and degree of bother.
Discussion
There is no formal evidence regarding the effects of history and physical exam on outcomes of IPT treatments however, there is universal agreement that taking a history and performing a physical examination should be the first step in the assessment of anyone with urinary incontinence.73 There is strong evidence that a history of pelvic RT74,75 is associated with the severity of incontinence, especially stress incontinence,76,77 after prostate surgery.
The Panel believes that before treating IPT, it is critical to categorize the type of incontinence and the severity and degree of bother of incontinence. The status of prostate cancer also should be known, particularly for men who are candidates for salvage RT, which may impact efficacy of continence treatment.
History is the first step in determining the type of incontinence, which is important because treatments for SUI and urgency incontinence are very different. In cases of mixed incontinence, it can be important to determine which component is more prevalent and bothersome, though many investigators feel that treatment outcomes for urgency incontinence may be difficult to determine in the face of significant sphincteric insufficiency.
Guideline Statement 10
Discussion
You May Like: How To Fix A Swollen Prostate
Management Of Bowel Dysfunction
Short of treating individual symptoms as needed, there are few, if any, treatment options for bowel dysfunction following radiation therapy. Laser therapy can stop rectal bleeding caused by radiation. Anti-diarrheal agents can help with loose bowel movements. Increasing fiber intake through whole grains, fruits and vegetables, or fiber supplements can also help.Avoiding foods that might irritate the gastrointestinal tract is important, but complete elimination of fibrous, bulky foods can lead to constipation and straining, which in turn can exacerbate rectal bleeding.
Benefits And What To Expect
The mission of the GRI is to ensure that our hand-selected team is comprised of the worlds best and brightest medical staff. With that in mind, we have built a team of over 50 professionals who strive to serve our patients and support the surgical teams pursuit of excellence. We have assembled a comprehensive team to deliver the best option to each patient that comes to our Institute. We take a multi-modality and multi-disciplinary approach to patient care, collaborating with experts in radiation oncology, medical oncology and internal medicine to provide the optimal comprehensive approach to urologic cancer to our patients. Surgery is not the best option for all patients therefore, we evaluate each patient individually and assess the potential prostate treatment options of active surveillance, radiation therapy, androgen deprivation and other surgical modalities.
The state-of-the art facilities at AdventHealth are unparalleled. From the resort inspired facility at Celebration Health to the hub of Central Florida’s healthcare at AdventHealth Orlando, patients travel from all over the globe to receive their treatment at our hospital. Fine dining, hotels and entertainment abound in Orlando, and patients and families often extend their stay in Orlando to take advantage of these amenities.
Read Also: Stage Four Prostate Cancer Prognosis
Peer Review And Document Approval
An integral part of the guideline development process at the AUA is external peer review. The AUA conducted a thorough peer review process to ensure that the document was reviewed by experts in the treatment of IPT. In addition to reviewers from the AUA PGC, Science and Quality Council , and Board of Directors , the document was reviewed by representatives from AUA and SUFU as well as external content experts. Additionally, a call for reviewers was placed on the AUA website from January 14-28, 2019 to allow any additional interested parties to request a copy of the document for review. The guideline was also sent to the Urology Care Foundation to open the document further to the patient perspective. The draft guideline document was distributed to 49 external peer reviewers. All peer review comments were blinded and sent to the Panel for review. In total, 33 reviewers provided comments. At the end of the peer review process, a total of 476 comments were received. Following comment discussion, the Panel revised the draft as needed. Once finalized, the guideline was submitted for approval to the AUA PGC, SQC and BOD as well as the governing bodies of SUFU for final approval.
Comparing Robotics Vs Open Continence Outcomes
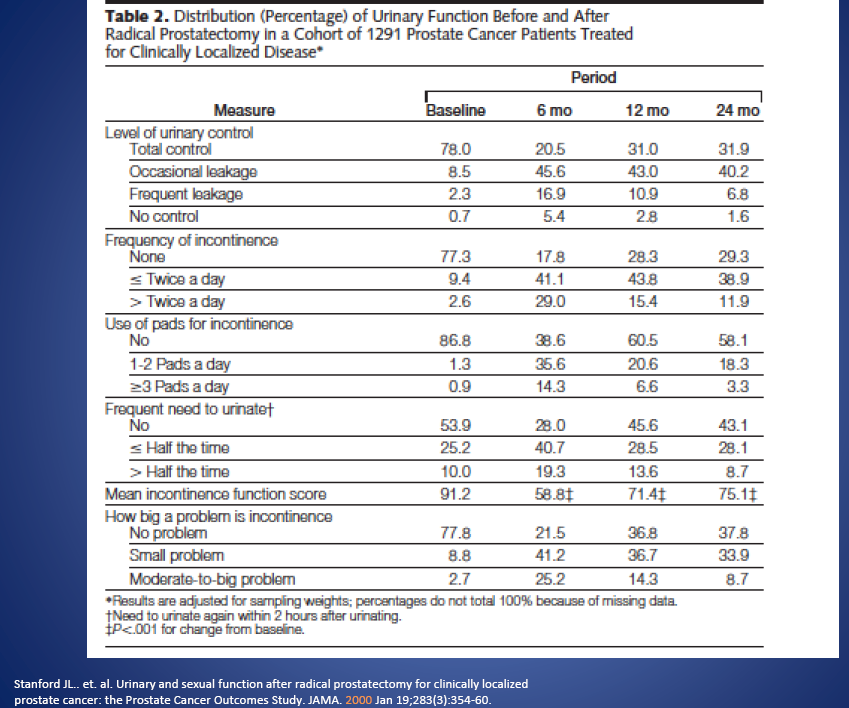
There are few head-to-head comparisons of open versus robotic surgery performed by the same surgeon at the similar points in their learning curve or case experience. It would be easy to skew the comparison in favor of the robotic camp by cherry-picking a handful of favorable robotics series and several low quality open radical prostatectomy studies. It is more informative to take an honest look at all of the available literature and analyze the outcomes data from the highest quality available studies from the top robotic and open surgeons. When analyzing these data from high volume surgeons where the technique from case to case is nearly identical, we have technical data so-to-speak, that is, data which is more influenced by surgical modality and operative technique than by patient factors. We must also review, however, bread-and-butter studies, which are more representative of the experience the average patient will have in a general community surgeon practice. The reality is that many patients are not having their operation done at the high volume academic centers from the top tier surgeons who are writing the papers from which we are extracting this data.
Don’t Miss: What Does Low Grade Prostate Cancer Mean
About Your Prostate Surgery
A radical prostatectomy is a surgery to remove your entire prostate gland and seminal vesicles. Some of the lymph nodes in your pelvis are removed as well. This is done to prevent cancer from spreading from your prostate to other parts of your body.
A radical prostatectomy can be done in 1 of 2 ways. One way is through an open incision , which is called an open prostatectomy. Another way is to use a laparoscope, which is a tube-like instrument with a camera. Your surgeon will talk with you about the best surgery option for you.
Open prostatectomy
In an open prostatectomy, your surgeon will make an incision that goes from your pubic bone towards your belly button . Theyll remove the pelvic lymph nodes first, followed by the prostate gland, and then the structures next to it.
Figure 2. Open prostatectomy incisions
Laparoscopic or robotic-assisted prostatectomy
During a laparoscopic or robotic-assisted prostatectomy, your surgeon will make several small incisions in your abdomen . Theyll insert a laparoscope into 1 of the incisions and use gas to expand your abdomen. Surgical instruments will be inserted into the other incisions to remove the prostate. Some surgeons at MSK are specially trained to use a robotic device to assist with this procedure.
Figure 3. Laparoscopic or robotic-assisted prostatectomy incisions
Measurement Of Membranous Urethral Length
MRI is the gold standard for measuring MUL. The clear visualization and cross-referencing of standard sagittal, axial and coronal T2-weighted MR images enables the identification of the apex of the prostate, membranous urethra and penile bulb,. However, obtaining preoperative MUL measurements using MRI is not routine in urological practices outside of large-volume centres. MRI investigations are costly, time consuming and resource intensive, requiring specialist technicians and radiologists to perform and evaluate the images. Furthermore, not all patients can undergo MRI owing to claustrophobia or the presence of metal implants. However, a 2018 investigation reported that preoperative MUL can be accurately and reliably measured by transperineal ultrasonography . In this study, transperineal ultrasonography-measured MUL demonstrated excellent agreement with MRI measurements , excellent testretest reliability and minimal difference between the two supine position measurements . Visualization of the MUL in the same patient using transperineal ultrasonography and MRI illustrates the excellent agreement between the two measurements .
Recommended Reading: Foods That Aggravate The Prostate
A Patients Story: Overcoming Incontinence
Christopher Miller* is a real estate agent who is married and has two sons. About five years ago, at age 56, Mr. Miller was diagnosed with prostate cancer. After a great deal of research and consultations with five doctors, Mr. Miller decided to have a radical prostatectomy.
Although he considers the operation a success, in that it has apparently eradicated the cancer, Mr. Miller struggled for almost two years to overcome persistent urinary incontinence. For much of that time, he felt ill-served by the medical community. The story of how he eventually overcame this problem may be helpful to other men in the same situation.
What was going through your mind when you learned you had prostate cancer?
Like anyone else, I was surprised. You never think its going to happen to you. The biggest fear, of course, is that it might be life-threatening. Even though I knew this is generally a disease that takes a long time to grow, I still wondered how much longer I might have to live. So I thought of things like: Is my family provided for? Are my financial affairs in order? Will my children be secure? Will I ever meet my grandchildren?
Of course, I was very concerned about my wife. Wed been married 32 years at that point, and I worried about what impact this would have on her. Shes a very strong and good person, and she remained at my side every moment of the time. And that support proved to be invaluable.
Why did you decide on a radical prostatectomy?
What Should I Do After Radiation Therapy To Reduce Incontinence
After radiation therapy, men should continue with the daily pelvic floor exercises they performed after their prostatectomy. Pelvic floor exercises help strengthen the muscles at your bladder outlet, which helps to improve, regain, or maintain bladder and bowel control.
To identify your pelvic floor muscles, stop urination in midstream or tighten the muscles that keep you from passing gas. If you tighten your pelvic floor muscles while looking in the mirror, the base of your penis will move closer to your belly and your testicles will rise. Do not tighten the muscles in your belly, thighs, or buttocks.
Once you have identified the muscles, aim to perform 3-10 sets of 10 repetitions every day. Some sets should be with long muscle contractions and others with quick muscle contractions:
- Long contractions: Slowly increase the time you can hold the contraction until you can hold for 10 seconds. Rest for 10 seconds between each contraction.
- Quick contractions: Quickly tighten then relax the muscles.
You May Like: What Vitamins To Take For Prostate Health
Problems After Prostate Cancer Treatment
Many men get urinary problems as a side effect of their treatment. This is because prostate cancer treatment can damage the nerves and muscles that control when you urinate .
If youre starting treatment for prostate cancer, ask your doctor about the possible side effects. Each treatment can cause different urinary problems. Your chances of getting each side effect will depend on the treatment youre having, and on whether or not you had urinary problems before starting treatment.
If youve already had prostate cancer treatment and you have urinary problems, tell your doctor or nurse. They can suggest treatments and lifestyle changes to help manage them.
Depending on the type of problems youre having, ways to manage them can include lifestyle changes, pelvic floor muscle exercises, bladder retraining, medicines or surgery. For practical tips read our How to manage urinary problems guide.
Watch Paul’s story below for one man’s experience of managing urinary problems after prostate cancer treatment.
Managing Incontinence After Robotic Prostatectomy
- On April 19, 2018
- 0 Comments
The popularity of the Robotic Prostatectomy has increased rapidly since its introduction in 2000.
As stated on the UCLA Health website, robotic prostatectomy offers a minimally invasive treatment with less blood and a rapid overall recovery. It is generally thought to be an accurate and precise method for removing
Also Check: Self Check Prostate Health Test