What Is The Immune System
Your immune system is made up of various organs, antibodies and immune cells that work together to fight disease and infections. Immune cells include:
- B-cell lymphocytes: These white blood cells produce infection-fighting antibodies.
- T-cell lymphocytes: These white blood cells target and destroy diseased cells. T-cells also alert other cells to the presence of diseased or foreign cells.
- Dendritic cells: These immune cells interact with T-cells to stimulate an immune system response.
- Granulocytes: These white blood cells neutrophils, eosinophils and basophils fight infections.
Inflammatory Responses In The Prostate
Inflammation is an innate response to harmful stimuli, such as infections, tissue damage, or tissue malfunction . The main goal with the inflammatory process is to clear the potential threat and restore tissue homeostasis. This normally occurs in two phases the recognition and elimination phase and the resolution and repair phase . If the acute response fails in eliminating the inflammatory agents, the inflammation shifts toward a chronic state. Instead of initiating the resolution phase, additional macrophages and lymphocytes are recruited and, depending on the inflammatory inducer, act to remodel the local microenvironment to adapt to an altered tissue homeostasis.
Cancer has been described as a wound that refuses to heal , and today many cancers have been tightly correlated with preceding inflammatory responses . Several lines of evidence support the theory that inflammation also precedes PCa . Proliferative inflammatory atrophy lesions are areas in the prostate with an increased infiltration of inflammatory cells. These regions can merge with prostatic intraepithelial neoplasia, which is considered to be a risk factor for the development of PCa . Also, a correlation with regular intake of non-steroidal anti-inflammatory drugs and reduced PCa risk has been observed .
The Grade Group And Psa Level Are Used To Stage Prostate Cancer
The stage of the cancer is based on the results of the staging and diagnostic tests, including the prostate-specific antigen test and the Grade Group. The tissue samples removed during the biopsy are used to find out the Gleason score. The Gleason score ranges from 2 to 10 and describes how different the cancer cells look from normal cells under a microscope and how likely it is that the tumor will spread. The lower the number, the more cancer cells look like normal cells and are likely to grow and spread slowly.
The Grade Group depends on the Gleason score. See the General Information section for more information about the Gleason score.
- Grade Group 1 is a Gleason score of 6 or less.
- Grade Group 2 or 3 is a Gleason score of 7.
- Grade Group 4 is a Gleason score 8.
- Grade Group 5 is a Gleason score of 9 or 10.
The PSA test measures the level of PSA in the blood. PSA is a substance made by the prostate that may be found in an increased amount in the blood of men who have prostate cancer.
Read Also: Can A Prostate Biopsy Spread Cancer
Side Effects Of Parp Inhibitors
Side effects of these drugs can include nausea, vomiting, diarrhea, fatigue, loss of appetite, low red blood cell counts , constipation, skin rash, abnormal liver blood tests, low blood platelet counts, cough and shortness of breath. Rarely, some people treated with these drugs have developed a blood cancer, such as myelodysplastic syndrome or acute myeloid leukemia. Some men taking olaparib had problems with blood clots in the lungs or legs.
Chimeric Antigen Receptor T
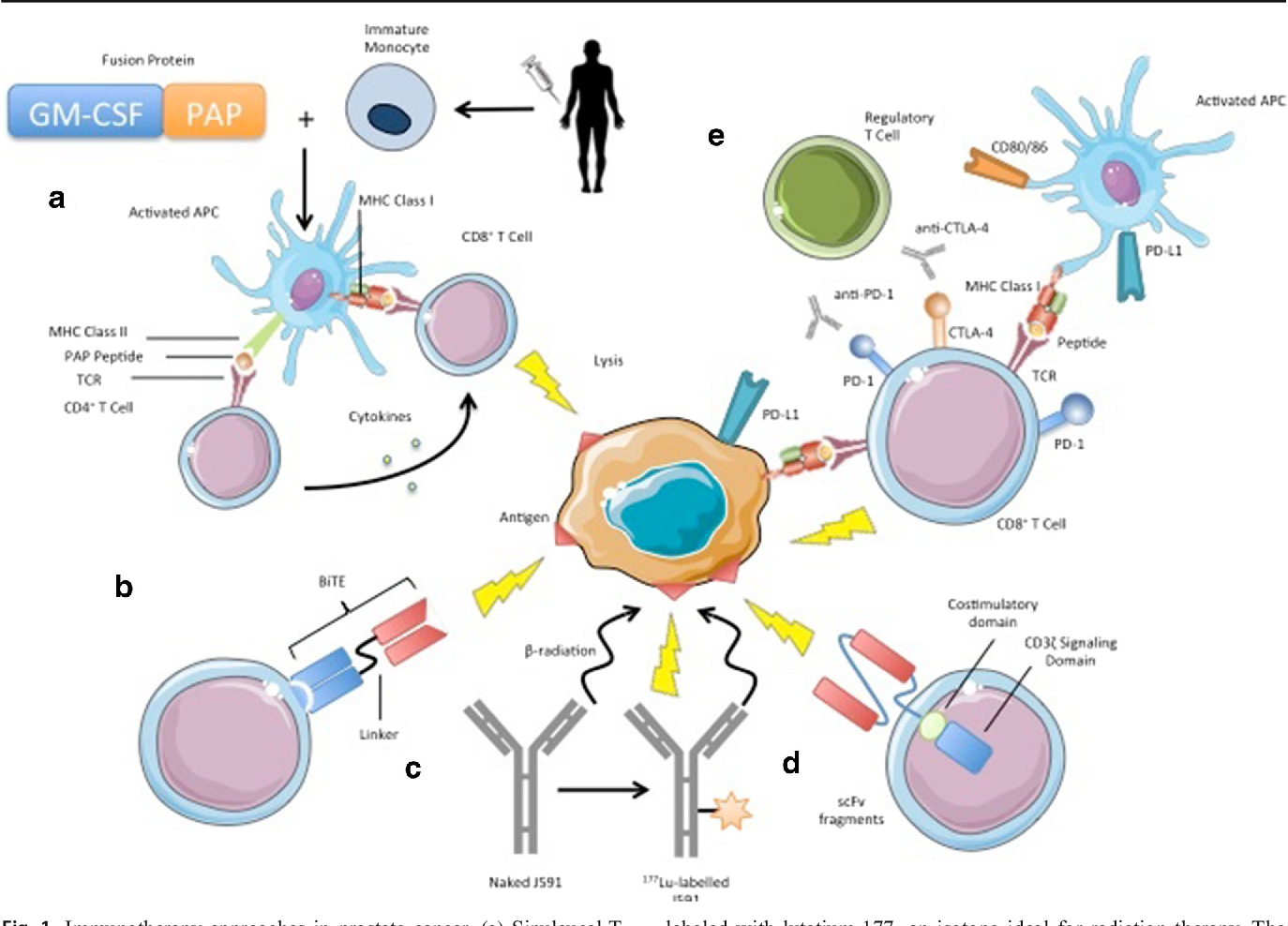
Another emerging field that has shown promise is chimeric antigen receptor T-cell therapy. CAR-T therapy involves taking a patients T cells, engineering them to express a T cell receptor directed against a certain antigen, expanding the cells, and reinfusing them back into the patient. CAR-Ts directed against CD19 have been approved for the treatment of relapsed/refractory acute lymphoblastic leukemia and diffuse large B-cell lymphoma. CAR-Ts are also designed to express costimulatory domains, which may interact with ligands or receptors on antigen-presenting cells, tumor cells, or on the T cell itself .
Also Check: Treatment Plan For Prostate Cancer
Combination Immunotherapy Benefits Subset Of Patients With Advancedprostate Cancer
Phase II trial provides rationale for pursuing further study of dualcheckpoint blockade
MD Anderson News ReleaseSeptember 10, 2020
Results from a Phase II trial led by researchers at The University of Texas MD Anderson Cancer Center suggest that a combination of ipilimumab plus nivolumab can generate durable responses in a subset of patients with metastatic castration-resistant prostate cancer , an immune-cold cancer that does not typically respond well to immunotherapy.
In a cohort of patients without previous chemotherapy treatment, the overall response rate was 25% and median overall survival was 19 months. In a post-chemotherapy cohort, the ORR was 10% and media OS was 15.2 months. Four patients achieved a complete response.
The results of the CheckMate 650 trial, published today in Cancer Cell, are the first report of combination immune checkpoint inhibitors in mCRPC. Early results from this study were presented at the 2019 American Society of Clinical Oncology Genitourinary Cancers Symposium. Based on the findings, alternate dosing regimens are now being evaluated in an expanded clinical trial to reduce treatment-related toxicities.
Designing a combination strategy
This would explain why previous clinical trials evaluating single-agent checkpoint inhibitors have not been effective in treating patients with mCRPC, said Sharma, who co-directs MD Andersons immunotherapy platform, part of the institutions Moon Shots Program®.
What Does Immunotherapy Treat
Immunotherapy treats different types of cancers , including but not limited to
- Bladder cancer.
- Cervical cancer and ovarian cancer.
- Colorectal cancer.
- Kidney cancer, liver cancer and lung cancer.
- Leukemia.
- Lymphoma
The main types of immunotherapy that healthcare providers use to treat cancer include:
- Adoptive cell therapy: Healthcare providers remove, change and then reintroduce a persons modified immune cells into the body. The modified cells seek out and destroy cancer cells. CAR T-cell therapy modifies T-cells with chimeric antigen receptors that fight cancer. Other therapies include natural killer cells and tumor-infiltrating lymphocytes .
- Cancer vaccines: Vaccines stimulate an immune response to protect the body against certain diseases. The human papillomavirus vaccine protects against an infectious disease that causes cervical, anal, throat and penile cancers. Theres also a vaccine for hepatitis B, which causes liver cancer.
- Immunomodulators: These substances change the bodys biologic response. They stimulate the immune systems ability to find and kill cancer cells. Treatments include checkpoint inhibitors, cytokines, interferon and interleukins.
- Monoclonal antibodies: These lab-made proteins attack specific parts of a cancer cell. Monoclonal antibodies can also deliver drugs, toxins or radioactive material directly to tumors.
- Oncolytic viruses: Specialists change these viruses in the laboratory. The modified viruses infect and kill cancer cells.
You May Like: What Happens When They Remove The Prostate
What Are The Types Of Immunotherapy
Several types of immunotherapy are used to treat cancer. These include:
- Immune checkpoint inhibitors, which are drugs that block immune checkpoints. These checkpoints are a normal part of the immune system and keep immune responses from being too strong. By blocking them, these drugs allow immune cells to respond more strongly to cancer.
-
Learn more about immune system modulators.
Support Programs And Services
All cancer patients at Mount Sinai have access to specialized support programs and services. These services include palliative care, treatment for pain, and integrative medicine. Integrative medicine involves using complementary and traditional medicine together. Our social workers, psychiatrists, dietitians, chaplains, and experts in palliative care are here to help. We focus on you with individual needs that may change over time. We work with you and your loved ones to evaluate your concerns and develop a personal plan. This plan may include counseling, practical help, education, symptom management, and wellness programs.
Don’t Miss: Prognosis Of Prostate Cancer Spread To Bones
Conflict Of Interest Statement
Harm Westdorp, Annette E. Sköld, Berit A. Snijer, Sebastian Franik, Sasja F. Mulder, Pierre P. Major, Ronan Foley, and I. Jolanda M. de Vries declare no disclosures of potential conflicts of interest. Winald R. Gerritsen is a consult for Aglaia Biomedical Ventures, is on the supervisory board for PsytoBe, has received speakers fee from J& J and BMS, and is on the advisory boards for Amgen, BMS, Janssen-Cilag, Sanofi, Astellas, Bayer, and Merck.
Hormone Therapy And Immunotherapy
Androgen-deprivation therapy affects the immune system by inducing thymic regeneration leading to increased production of naive T cells , decreasing CD4+ T-cell tolerance , and increasing CD4+ effector T cells . The synergistic effect of castration and immunotherapy has been evaluated in multiple clinical trials .
Antiandrogens such as enzalutamide also induce immunogenic modulation . Enzalutamide is currently being tested in combination with PROSTVAC in mCRPC and in biochemical recurrence . Interestingly, mCRPC patients who progressed on enzalutamide were shown to have increased expression of PD-1 in circulating immune cells . Graff et al. reported a case series of 10 mCRPC patients enrolled in a phase II trial of pembrolizumab after progression on enzalutamide. Three out of 10 patients had rapid PSA declines and 2 had PRs, including one patient with MSI . KEYNOTE-365 is currently investigating pembrolizumab combination therapies in mCRPC, including pembrolizumab + olaparib, pembrolizumab + docetaxel + prednisone, and pembrolizumab + enzalutamide .
You May Like: Rotterdam Prostate Cancer Risk Calculator
Targeted Immunotherapy For Deadly Prostate Cancer Shows Promise In Preclinical Test
Using a targeting molecule to concentrate toxic chemotherapy in tumors could hold potential as a treatment for an aggressive subtype of advanced prostate cancer, according to work published November 16 in the journal Clinical Cancer Research. Scientists at Fred Hutchinson Cancer Research Center show that some neuroendocrine prostate cancer cells have high levels of a specific protein marker, and that using this marker to guide chemotherapy to these cancer cells eradicates human tumors growing in mice.
âWeâre developing a targeted treatment for a disease that otherwise didnât have any targeted treatments. Thatâs huge,â said Hutch prostate cancer researcher Dr. John Lee, the paperâs senior author. âIt takes into account that not all cancers of a specific tissue are the same. You really have to delve deeper to understand how one personâs disease may be different from anotherâs.â
He is working with Immunomedics, Inc., the manufacturer of the experimental therapy and now a subsidiary of Gilead Sciences, Inc., to initiate an early stage clinical trial in patients with neuroendocrine prostate cancer. Lee and his team have no financial stake in the potential treatment.
The experimental drug is an antibody-drug conjugate, in which a drug is attached to an antibody, a specialized immune protein that can bind to other proteins. Scientists have modified them to carry cancer-killing drugs to specific cellular targets.
Rationale For The Use Of Immunotherapy In Prostate Cancer
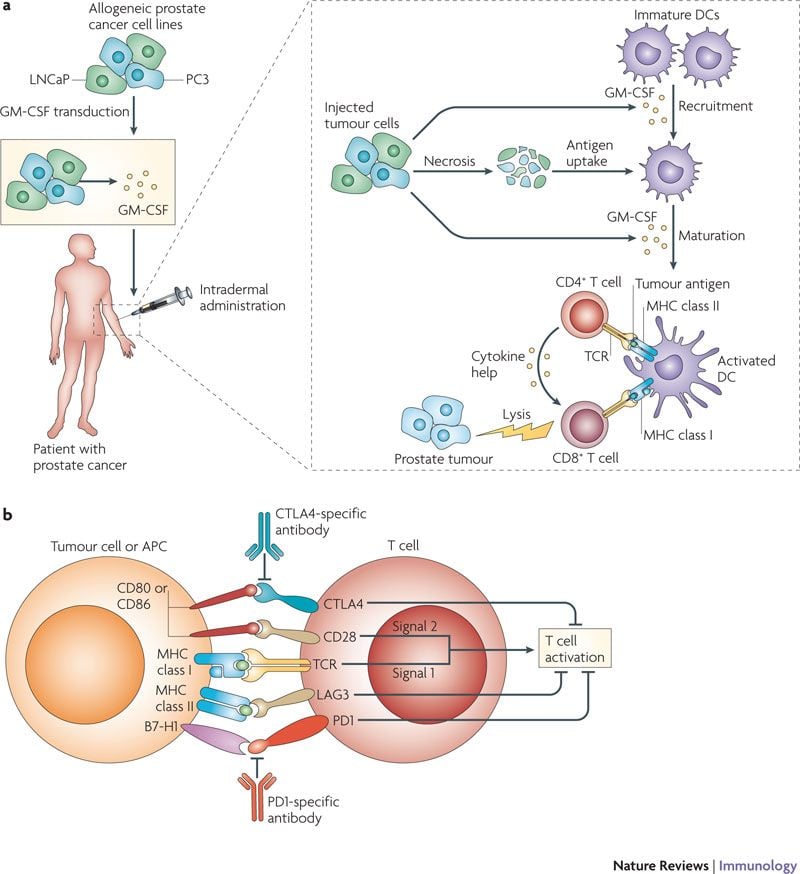
Sipuleucel-T , an autologous cellular immunotherapy, was approved by the U.S. Food and Drug Administration in 2010 for treatment of patients with asymptomatic or minimally symptomatic mCRPC. A pivotal phase III clinical trial randomized 512 mCRPC patients 2:1 to receive sipuleucel-T or placebo. This positive study had a median overall survival of 25.8 vs. 21.7 months , and no significant difference in time to progression . The toxicity profile was good, with transient flu-like symptoms and fever as being the most common side effects .
To receive this therapeutic cancer vaccine, patients first undergo leukapheresis to obtain autologous peripheral blood mononuclear cells . The PBMCs are activated with a recombinant protein consisting of prostatic acid phosphatase and GM-CSF, then reinfused after 3 days. This process is repeated every 2 weeks for 3 doses. Although the exact mechanism of action of sipuleucel-T is not known, this treatment does not decrease prostate-specific antigen levels or tumor size but does prolong OS, likely by affecting tumor growth . Interestingly, sipuleucel-T treatment resulted in humoral antigen spread, including development of antibodies to ERAS, KLK2, and KRAS, that was associated with improved OS . The Society for Immunotherapy of Cancer Consensus Recommendations indicate that sipuleucel-T vaccine should be considered early in the treatment of mCRPC, since doing so appears to have a greater OS benefit .
Recommended Reading: How Do People Get Prostate Cancer
Vaccines And Checkpoint Inhibitors
Preclinical studies have suggested that different therapeutic cancer vaccine platforms can activate different T-cell populations, even if they target the same antigens , and that the combination of cancer vaccines and checkpoint inhibitors has synergistic effects . Ideally, cancer vaccines should activate immune cells and direct them to the tumor , where they can increase lymphocyte infiltration and drive increased PD-L1 expression within the tumor microenvironment. One of the major concerns with this approach has been the possibility of increased toxicity however, preliminary data suggest that this combination is no more toxic than a single-agent checkpoint inhibitor . Consequently, a vaccine plus a PD-1 inhibitor may be less toxic than a vaccine plus a CTLA-4 inhibitor.
A phase I trial evaluated the combination of GVAX , a whole tumor-cell vaccine, and ipilimumab in mCRPC. Seven of 28 patients had > 50% PSA declines, while one patient had a complete response . Another study treated 30 patients, 24 of whom were chemotherapy-naïve, with PROSTVAC and ipilimumab. Six of the 30 patients had PSA declines > 50%. The median OS was 34.4 months, and 2-year OS was 73%, which was better than historical controls .
A phase I/II study of a Listeria-vector vaccine plus pembrolizumab is currently accruing patients with mCRPC . Another phase II study will evaluate the combination of PROSTVAC, ipilimumab, and nivolumab in prostate cancer patients prior to curative surgery .
Microbial Vectors For Cancer Immunotherapy
The ability of microbial vectors to carry foreign antigens has been harnessed by various vaccine approaches to targeted immunotherapy. Bacterial strains have been engineered to express cancer-specific antigens and cytokines, as well as prodrug-converting cytokines. A variety of microbial vectorsincluding BCG, Listeria monocytogenes , Salmonella, Escherichia coli, and Shigellahave demonstrated efficacy as vaccine vectors in preclinical animal models of infectious disease and cancer. These microbial vectors are useful because of their strong ability to infect APCs and induce potent antitumour responses to targeted antigens. However, utilization of microbial agents as delivery vehicles is limited because the properties of these vaccine vectors have not yet been fully characterized.
Don’t Miss: Can You Get An Erection After Prostate Surgery
How Effective Is Immunotherapy
Success rates for any cancer treatment, including immunotherapy, depend on individual factors, including the cancer type and stage. In general, immunotherapy is effective against many cancers. While some cancers are more immunogenic than others, in general, immunotherapy is effective across a wide variety of cancers. Immunotherapy can produce durable responses unlike chemotherapy or radiation, however, these occur only in around 25% patients.
Some research suggests that the immune system may remember cancer cells after immunotherapy ends.
Remission And The Chance Of Recurrence
A remission is when cancer cannot be detected in the body and there are no symptoms. This may also be called having no evidence of disease or NED.
A remission can be temporary or permanent. This uncertainty causes many people to worry that the cancer will come back. Although there are treatments to help prevent a recurrence, such as hormonal therapy and radiation therapy, it is important to talk with your doctor about the possibility of the cancer returning. There are tools your doctor can use, called nomograms, to estimate someone’s risk of recurrence. Understanding your risk of recurrence and the treatment options may help you feel more prepared if the cancer does return. Learn more about coping with the fear of recurrence.
In general, following surgery or radiation therapy, the PSA level in the blood usually drops. If the PSA level starts to rise again, it may be a sign that the cancer has come back. If the cancer returns after the original treatment, it is called recurrent cancer.
When this occurs, a new cycle of testing will begin again to learn as much as possible about the recurrence, including where the recurrence is located. The cancer may come back in the prostate , in the tissues or lymph nodes near the prostate , or in another part of the body, such as the bones, lungs, or liver . Sometimes the doctor cannot find a tumor even though the PSA level has increased. This is known as a PSA-only or biochemical recurrence.
Also Check: What Is The Psa Test For Prostate
Moffitts Approach To Prostate Cancer Immunotherapy
Moffitt Cancer Center is a National Cancer Institute-designated Comprehensive Cancer Center the only Comprehensive Cancer Center based in Florida. This designation reflects our dedication to both clinical excellence and research efforts. Our team is continually working on groundbreaking immunotherapy treatments for all types of cancer, including prostate cancer. Our robust clinical trials program is constantly evolving.
Moffitt takes a multispecialty approach to prostate cancer treatment, which means that our team includes all types of physicians surgeons, medical oncologists, radiation oncologists and more and all of them are trained in the treatment of prostate cancer, specifically. Individualized treatment plans are developed collaboratively, with all elements working together to yield the best results and a higher quality of life for our patients.
To learn more about immunotherapy for prostate cancer or to speak with an oncologist specializing in prostate cancer treatment, call or fill out our new patient registration form online. New patients are welcome to visit Moffitt with or without a referral.
- BROWSE
Certain Factors Affect Prognosis And Treatment Options
The prognosis and treatment options depend on the following:
- The stage of the cancer .
- The patients age.
- Whether the cancer has just been diagnosed or has recurred .
Treatment options also may depend on the following:
- Whether the patient has other health problems.
- The expected side effects of treatment.
- Past treatment for prostate cancer.
- The wishes of the patient.
Most men diagnosed with prostate cancer do not die of it.
Don’t Miss: Foods Good For Prostate Cancer
A Biopsy Is Done To Diagnose Prostate Cancer And Find Out The Grade Of The Cancer
A transrectal biopsy is used to diagnose prostate cancer. A transrectal biopsy is the removal of tissue from the prostate by inserting a thin needle through the rectum and into the prostate. This procedure may be done using transrectal ultrasound or transrectal MRI to help guide where samples of tissue are taken from. A pathologist views the tissue under a microscope to look for cancer cells.
Sometimes a biopsy is done using a sample of tissue that was removed during a transurethral resection of the prostate to treat benign prostatic hyperplasia.
If cancer is found, the pathologist will give the cancer a grade. The grade of the cancer describes how abnormal the cancer cells look under a microscope and how quickly the cancer is likely to grow and spread. The grade of the cancer is called the Gleason score.
To give the cancer a grade, the pathologist checks the prostate tissue samples to see how much the tumor tissue is like the normal prostate tissue and to find the two main cell patterns. The primary pattern describes the most common tissue pattern, and the secondary pattern describes the next most common pattern. Each pattern is given a grade from 3 to 5, with grade 3 looking the most like normal prostate tissue and grade 5 looking the most abnormal. The two grades are then added to get a Gleason score.