The Upoint Clinical Phenotyping System For Cpps
The most widely adopted questionnaire for clinical evaluation of CPPS is the National Institutes of Health Chronic Prostatitis Symptom Index .16 This tool, validated in 1999, is composed of nine different questions investigating pain, urinary symptoms, and QoL related to CPPS. In 2009, Shoskes et al17 proposed a dedicated clinical classification of CPPS, to separately identify the different possible reported symptoms. It considers: Urinary symptoms Psychosocial dysfunction Organ-specific findings Infection Neurological/systemic and Tenderness of muscles .
The understanding of this clinical phenotyping system for CP/CPPS can explain why this disease has a wide multifactorial genesis, potentially different in each patient, therefore generating an individual multifaceted complex of symptoms for every patient diagnosed with CP/CPPS. A review by Magistro et al23 analyzed 28 randomized controlled trials evaluating various treatments for CP/CPPS, and underlined that monotherapy is never enough to achieve symptom relief and that the therapeutic approach should focus on the different symptomatic pattern presented by the patient in a multimodal setting.
Back Pain Can Actually Be Caused By Prostate Cancer And By The Time This Happens The Cancer Has Spread It Is At An Advanced Stage
In general, prostate cancer causes no symptoms, begins Kenneth Peters, MD, chief of urology for Beaumont Hospital, Royal Oak, MI.
Dr. Peters continues, In advanced cases, the cancer can metastasize to the bones, leading to back pain. Urinary retention or incomplete emptying of the bladder due to an enlarged prostate can at times be perceived as low back pain.
Low back pain has many possible causes, and there are different kinds of LBP, in that it can present in different ways.
Sometimes its accompanied by tingling or numbness radiating down a leg.
Sometimes LBP occurs only when you are in certain body positions, such as bending over, or standing up after sitting for long periods.
And there are people for whom LBP occurs only in the morning after getting out of bed, then dissipates soon after.
Sometimes low back pain is nearly constant but dull in nature.
The persistence is something to be concerned about, even if the level of pain is dull.
If youve been experiencing low back pain and it doesnt seem to be related to certain body positions and/or has not gone away after a week or two, do not blow this off.
Rather, bring this to the attention of your doctor and ask that your prostate be examined and that cancer be ruled out.
Dr. Peters, in practice for 30+ years, is board certified by the American Board of Urology. One of his specialties is treating bladder pain.
Copyright Notice
Disclaimer
Website Advertising Disclaimer
Dealing With Pain And Prostate Cancer
Until your pain is under control it may be very difficult to think clearly or believe that the pain will go away. Coping with any type of pain, whether it is constant or comes and goes, can be tiring and frightening. Pain can affect your daily activities, your relationships with other people, your sleep, and your ability to enjoy life.
Pain can also affect your thoughts and feelings. Theres no right way that youre supposed to feel and everyone reacts in their own way. You might feel scared, worried, stressed, helpless or even angry. Some people with pain say they feel angry or depressed. And some men worry that their pain is a sign that their cancer is getting worse.
Your feelings can also affect your pain anxiety can make it worse, and feeling low can make you more aware of your pain. It might be useful to get some extra help if youre feeling down, for example by talking to a counsellor.
Tiredness can also be a big problem if youre living with pain. If youre feeling very tired, speak to your GP or your doctor or nurse at the hospital. They can give you advice and support. Read more about extreme tiredness or find out about our fatigue support service.
There are things you can do to help yourself and people who can help.
Who can help?
Your medical team
Getting help at night or at the weekend , or in an emergency
Support from hospices
Recommended Reading: Hormone Replacement Therapy For Prostate Cancer
What Are Clinical Trials And Are They Right For You
Clinical trials are part of clinical research and at the heart of all medical advances. Clinical trials look at new ways to prevent, detect, or treat disease. Researchers also use clinical trials to look at other aspects of care, such as improving the quality of life for people with chronic illnesses. Find out if clinical trials are right for you.
What Should I Do If I Have Prostate Cancer Symptoms
If you are displaying one or more signs of prostate cancer, be sure to promptly consult with a physician. Even benign prostate conditions like prostate enlargement warrant timely medical attention, so dont delay seeking treatment. And, like most other malignancies, prostate cancer is usually more easily treated when it is detected at an early stage.
Don’t Miss: Is Coffee Bad For Prostate Cancer
When To Have Psa Tests
The prostate gland produces a protein called PSA. Levels of this protein increase when the prostate is dealing with irritation, swelling, or the growth of cancerous cells.
High levels of PSA in the blood do not necessarily mean that an individual has prostate cancer, but they can suggest that further tests are necessary.
The Prostate Cancer Research Institute recommend that most men start having PSA tests at the age of 45.
Males with a higher risk of developing the disease, including those who are African-American or who have a family history of prostate cancer, should start undergoing these tests at age 40.
Sex And The Prostate: Overcoming Erectile Dysfunction When You Have Prostate Disease
If you are concerned about erectile function, its important to understand what erectile dysfunction really is. Failing to have an erection one night after youve had several drinks or even for a week or more during a time of intense emotional stress is not erectile dysfunction. Nor is the inability to have another erection soon after an orgasm. Nearly every man occasionally has trouble getting an erection, and most partners understand that.
Erectile dysfunction is the inability to attain and maintain an erection sufficient for sexual intercourse at least 25% of the time. The penis doesnt get hard enough, or it gets hard but softens too soon. The problem often develops gradually. One night it may take longer or require more stimulation to get an erection. On another occasion, the erection may not be as firm as usual, or it may end before orgasm. When such difficulties occur regularly, its time to talk to your doctor.
Erectile dysfunction can have many causes, including some forms of prostate disease and medications and surgery for prostate cancer. Fortunately, in many cases, this problem can often be effectively addressed. Some men find relief by taking medications to treat erectile dysfunction. If these arent effective for you, a number of other options, including injections and vacuum devices, are available. The possibility of finding the right solution is now greater than ever.
You May Like: Bone Scan Vs Pet Scan For Prostate Cancer
Providing Your Medical History
At first, the doctor will probably ask you about your medical history. Do you have any chronic illnesses? What illnesses and operations have you had in the past? What medications are you taking, if any? Your doctor is also likely to ask about your psychological well-being and lifestyle: Do you suffer from depression? Are you under a lot of stress? Do you drink alcohol? Smoke? Use illegal drugs? Have you felt a loss of affection for your partner? Have you recently grown interested in a new partner?
As part of this health history, be prepared to tell your doctor specific details about the symptoms that brought you to the office and when they began. Your doctor might want to know how often you had sex before the problem started and if there have been weeks or months in the past when youve had erectile dysfunction. Your doctor may conduct a written or verbal screening test.
If the cause is clear a recent operation for prostate cancer, for example the conversation may move directly to your treatment options. Otherwise, you may need to answer more questions to help the doctor narrow down the possible causes and avoid unnecessary testing.
What Is Cauda Equina Syndrome
Cauda equina syndrome is a rare condition but has serious consequences if not treated promptly. It is most often caused by a large disc herniation in the lower back that compresses the nerve roots at the end of the spinal cord . These nerve roots are bundled together and resemble the tail of a horse. This is how they get their name. Cauda equina means “horse’s tail” in Latin.
Unlike most back problems that are longstanding or chronic, cauda equina is an acute event, like a stroke or heart attack. It most often develops rapidly, within as few as 6 to 10 hours. Classic symptoms of back pain, coupled with a sudden onset of numbness in the genital area and sudden urinary retention, are signs of a medical emergency. Relieving compression quickly can determine whether one resumes a normal life or lives with incontinence and paralysis of the legs.
Less often, in people with recurrent back problems, cauda equina can come on gradually, with a slow progression of urinary symptoms. Because cauda equina syndrome is a disorder of the nerves that control the bladder, its symptoms can be similar to those caused by bladder or prostate problems.
Read Also: Everything To Know About Prostate Cancer
What Is Prostate Cancer
Prostate cancer is common among American men. Your chance of getting prostate cancer may be affected by your:
- Age. Men age 50 and older run a greater risk.
- Race. Prostate cancer is most common among African-American men.
- Family history. If your father or brother has had prostate cancer, you are more likely to have it, too.
- Diet. Eating high-fat food with few fruits and vegetables may raise your risk.
When To Seek Medical Care
A person may have urinary symptoms unrelated to prostatitis that are caused by bladder problems, UTIs, or benign prostatic hyperplasia. Symptoms of prostatitis also can signal more serious conditions, including prostate cancer.
Men with symptoms of prostatitis should see a health care provider.
Men with the following symptoms should seek immediate medical care:
- complete inability to urinate
- great discomfort or pain in the lower abdomen and urinary tract
Read Also: Can I Shrink My Prostate
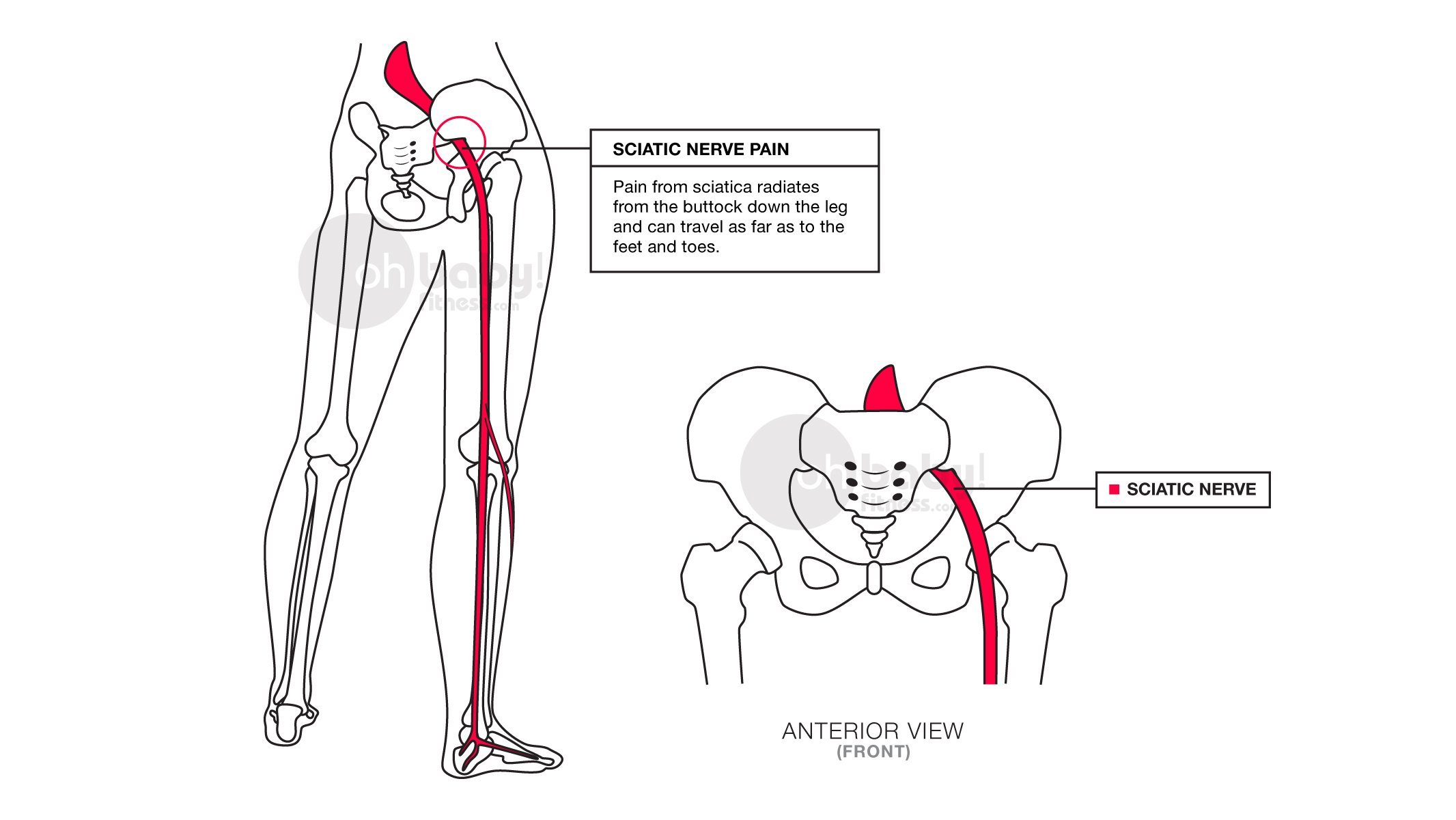
Is It Sciatica Or Peripheral Neuropathy What You Need To Know
The symptoms of sciatica or peripheral neuropathy are easy to confuse. Both conditions cause pain, numbness, and tingling in the legs and feet. The impact on your strength and balance may also make falls more likely.
Sciatica and peripheral neuropathy are two of the more challenging conditions treated at Algonquin Chiropractic. You may limit the activities you enjoy when you have one of these problems. You may also struggle to get a good nights sleep or turn to potentially addictive medicine.
The conditions are very different, however. Read on to learn more and find out how chiropractic care can help.
How Is Sciatica Diagnosed
Because of the specific type of pain sciatica causes, the team may diagnose sciatica based on your symptoms. To rule out other conditions that may cause this type of pain, they may order diagnostic imaging tests, like X-rays or an MRI, to check for other abnormalities in your lumbar or lower spine.
To assess the severity of your sciatica pain and your range of motion in your lower back, your physician may ask you to perform certain movements during a physical exam.
Once your doctor confirms sciatica, they will create a treatment plan to manage your pain and improve the overall health of your lumbar spine.
Read Also: Does Aspirin Help Enlarged Prostate
Prostatitis: Inflamed Prostate Can Be A Vexing Health Problem
- By Patrick J. Skerrett, Former Executive Editor, Harvard Health
When it comes to prostate trouble, the lions share of attention goes to prostate cancer and an enlarged prostate. A third condition, prostatitis, flies under the radar even though it affects up to one in six men at some point in their lifetimes. It triggers more than two million visits to doctors and untold agony each year.
Prostatitis, which means inflammation of the prostate gland, is an equal opportunity disorder. Unlike prostate cancer and benign prostatic hyperplasia , which predominantly affect older men, prostatitis affects men of all ages.
Prostatitis refers to a loose assemblage of syndromes characterized by urinary problems such as burning or painful urination, the urgent need to urinate, trouble voiding, difficult or painful ejaculation, and pain in the area between the scrotum and rectum or lower back. Although it causes some of the same symptoms as BPH and can occur at the same time, prostatitis is a separate condition.
Some types of prostatitis are caused by bacterial infection. These cases are often accompanied by the classic symptoms of infection, such as fever, chills, and muscle pain along with urinary problems. As a result, they are relatively easy to diagnose and treat, and they usually respond well to antibiotics. Unfortunately, such straightforward forms of prostatitis are the minority.
Causes And Related Problems
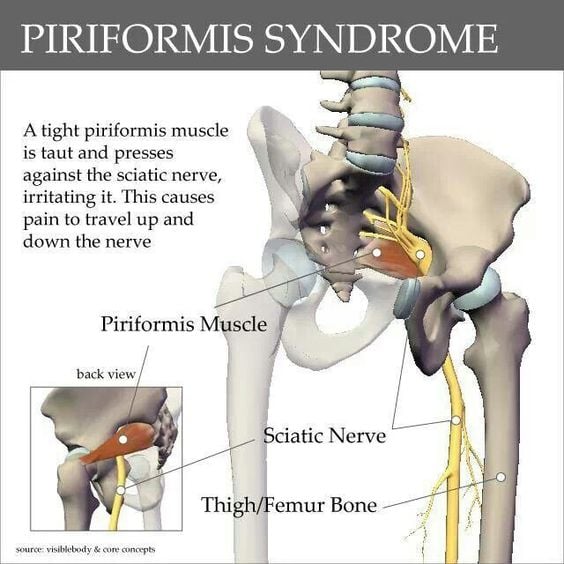
Nerve irritation or compression in the lower back most often cause sciatica. Back painis also common. Two other problems, herniated disc and spinal stenosis, may also play a role:
Doctors may order MRIs or EMGs to learn more. They may also recommend medicine, physical therapy, steroid injections, or surgery.
You May Like: What Are The Side Effects Of Prostate Radiation Therapy
Treatment For Rectal Discomfort
Since rectal discomfort can be due to a variety of causes, the exact treatment for the condition depends on the nature of the underlying cause. Therefore, treatments for rectal discomfort can vary widely on a case-to-case basis. Treatments may be done through medications, surgery, or just lifestyle changes. The severity of the symptoms of rectal discomfort do not always correlate with the seriousness of the underlying condition.
Mild symptoms may occur due to life-threatening conditions, whereas severe symptoms may not be due to any serious cause. Therefore, it is best to get the cause of rectal discomfort diagnosed by a qualified doctor. Regardless of the underlying cause of rectal discomfort, the following lifestyle measures may help in easing the discomfort:
- Avoid excessive wiping of the anal area when cleaning up after a bowel movement. Using a slightly wet toilet paper may prevent any abrasions during wiping.
- Avoid prolonged sitting in the toilet. Do not read or use mobile devices in the toilet as they are frequent contributors to the habit of sitting in the toilet for a long time.
- Use of sitz baths can provide relief from the symptoms of hemorrhoids.
- The anal area should be cleaned properly during bathing and dried thoroughly afterwards.
- Toilet papers should be soft and of good quality.
These measures do not replace medical treatments for rectal discomfort. Rather, they may help in preventing some cases of rectal discomfort.
Symptoms Of Prostate Cancer
Once a tumor causes your prostate gland to swell, or once cancer spreads beyond your prostate, you may have symptoms including:
- The need to pee often, especially at night
- Trouble starting or stopping a stream of urine
- A weak stream or one that starts and stops
- Leaking pee when you laugh or cough
- Not being able to pee standing up
- Pain or burning when you pee
- Pain or burning when you ejaculate
- Less fluid when you ejaculate
- Blood in your pee or semen
- Pressure or pain in your rectum
- Pain or stiffness in your lower back, hips, pelvis, or thighs
- New trouble getting an erection
These arenât symptoms of the cancer itself. They happen because the cancer growth is blocking your prostate.
Don’t Miss: Drugs For Metastatic Prostate Cancer
Differential Diagnosis With Pudendal Nerve Entrapment Syndrome
Originating from the sacral branches S2, S3, and S4, the pudendal nerve carries sensation from the external genitalia and the skin of the perineum and anus regions, as well as the motor supply to various pelvic muscles, including the male or female external urethral sphincter and the external anal sphincter. Its main branches are the superficial branch, with a sensitive innervation from the perineum and scrotum/labia region, and the deep branch, with a motor supply for bulbocavernosus, ischiocavernosus, superficial and deep transverse perineus, and sphincter urethrae muscles. The terminal branch of the PN is the dorsal nerve of the penis or clitoris. Therefore, this nerve is related to the entire pelvic and anogenital area, and its compression or irritation can lead to a wide variety of symptoms.
Pudendal neuralgia, also known as Alcocks canal syndrome, was first described by Amarenco et al in 1987, in a French paper.69 It may be related to or be secondary to childbirth, pelvic surgery, intense cycling, sacroiliac skeletal abnormalities, or age-related changes. The most well-known diagnostic criteria for PN are the Nantes criteria, first published in 2008.70 The diagnosis is mainly clinical, and its five main signs according to these criteria are: 1) pain in the anatomical territory of the PN , which is 2) worsened by sitting 3) symptoms do not wake the patient during the night 4) no objective sensory loss on clinical examination and 5) positive anesthetic PN block.
Who Is More Likely To Develop Prostatitis
The factors that affect a mans chances of developing prostatitis differ depending on the type.
Chronic prostatitis/chronic pelvic pain syndrome. Men with nerve damage in the lower urinary tract due to surgery or trauma may be more likely to develop chronic prostatitis/chronic pelvic pain syndrome. Psychological stress may also increase a mans chances of developing the condition.
Acute and chronic bacterial prostatitis. Men with lower UTIs may be more likely to develop bacterial prostatitis. UTIs that recur or are difficult to treat may lead to chronic bacterial prostatitis.
Don’t Miss: Preparation For Radiation Therapy For Prostate Cancer